Call Us Today!
(970) 247-2677
New Patients
(970) 233-7384
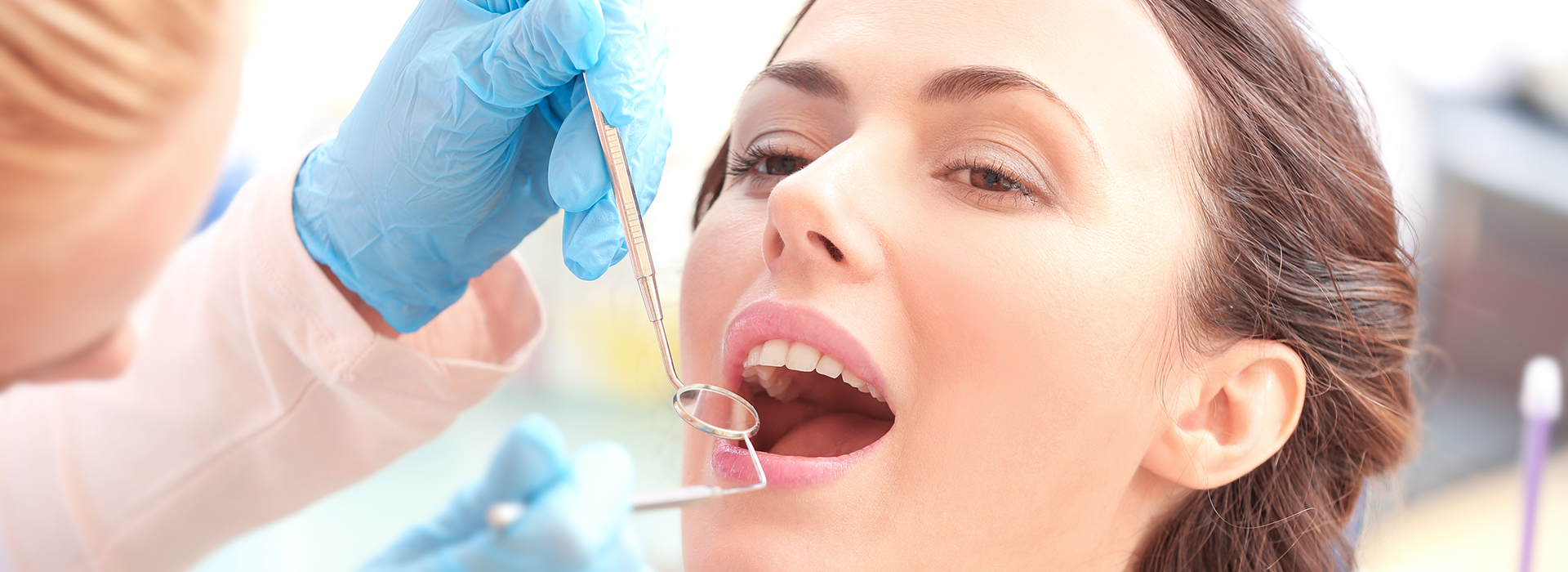
Did you know that the most common cause of tooth loss in adults is gum disease? According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease. However, the good news is that periodontal disease is almost entirely preventable. At the office of Mountain Health Dentistry, we offer a comprehensive range of services to help patients maintain optimal periodontal health and enjoy the benefits of a smile that look, feels, and functions at its best.
Periodontal disease, more commonly known as gum disease, is a set of inflammatory diseases that affect the "periodontium", which are the hard and soft tissues surrounding and supporting your teeth. Just like tooth decay, gum disease is attributed to the harmful bacteria in dental plaque and tartar that accumulate around the teeth and under the gums.
Since the progression of periodontal disease is often painless, you may not even be aware of an ongoing disease process. For this very reason, it’s essential to practice good oral hygiene and schedule visits for regular checkups, professional cleanings, and routine care.
Taking care of your smile includes being mindful of the signs and symptoms of gum disease.
Some indications that you may have periodontal disease include:
Inflamed and red gums
Bleeding when brushing or flossing
Receding gums and exposed tooth root surfaces
Sensitivity to hot or cold temperatures
Bad breath or a bad taste in the mouth
Teeth that feel loose
New spaces developing between the teeth or a change in the bite
Change in the fit of existing partial dentures
Discharge around the teeth and gums
Sharp or dull pain when biting down or chewing food

Taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, and respiratory problems.
At the office of Mountain Health Dentistry, we emphasize the importance of prevention, early detection, and timely treatment of periodontal disease. We provide patients the guidance, support, and care required to maintain optimal periodontal health.
Gingivitis represents the initial stage of gum disease. Although it doesn’t cause overt discomfort and often goes unnoticed, there are specific signs to be aware of that indicate the start of a problem. If you notice your gums bleed when you brush, look red and inflamed, or feel a little tender, you more than likely have gingivitis.
The good news is that by treating gingivitis early, the tissue damage associated with more advanced stages of gum disease can be avoided. Despite the presence of inflammation, the overall integrity of the periodontal tissues in this stage remains intact.
Treatment instituted at this point is often sufficient to reverse the course of the disease and to avoid any permanent damage to the periodontal tissues. A series of deep dental cleanings, an improved home care regimen and a commitment to regular maintenance may be all that is required to prevent this stage of periodontal disease from progressing.

When left untreated, a case of gingivitis develops into a more advanced and damaging stage of gum disease, known as periodontitis. At this point, the connective tissue and bone that hold the teeth in place begin to break down. With the progression of periodontal disease and periodontitis, more and more tissue loss ensues. Damage often includes an increase in pocketing between the teeth and bone, gum recession, and bone loss. As unresolved periodontitis goes from mild to moderate to severe, it increasingly compromises the soft and hard tissues supporting the teeth.
Periodontal treatment in this phase is designed to halt the progression of the disease and to restore tooth support as possible. Treatment may involve medications to control the bacteria and reduce the size of the pockets between the teeth and gums, gum surgery, as well as bone and tissue grafts.
At the office of Mountain Health Dentistry, we offer personalized, state-of-the-art solutions to help you maintain healthy gums and an attractive, well-functioning smile. As skilled providers of care, we utilize leading-edge technology and treatment methods to address a broad range of periodontal conditions and needs.
Thanks to advances in care, periodontal treatment today not only helps to halt the progression of gum disease but also delivers effective solutions, including bone grafting and regenerative procedures to repair tissue damage, restore bone volume, improve cosmetics, or provide adequate support for the placement of dental implants.
The type of periodontal treatment you receive depends on several factors including the stage of periodontal disease, the extent of tissue damage, your overall oral health, existing medical conditions, and other considerations in care. After a thorough assessment of your case, we’ll discuss your options to reestablish and maintain optimal periodontal health. We welcome your questions and are always on hand to provide guidance and address your concerns.
When periodontal disease is detected early in its onset, conservative or non-surgical methods of care combined with improved hygiene routines can restore periodontal health. While periodic, professional cleanings are sufficient to maintain periodontal health in patients that do not have gum disease, once gingivitis is present, deeper cleanings and possibly other non-surgical methods of care are recommended to treat the condition.
The American Academy of Periodontology emphasizes achieving periodontal health by means of the least invasive and cost-effective treatment approaches to care. Deeper cleanings, which include Scaling and Root planing, are non-surgical procedures that are considered the first line of defense against the progression of periodontal disease.
With scaling and root planing, any plaque and tartar (hardened dental plaque) that have accumulated below the gumline are carefully removed, and then the root surfaces of the teeth are smoothed. Since periodontal disease is an inflammatory response to plaque, tartar, and bacterial toxins, by simply mechanically eliminating these agents, the progression of gum disease can be halted. In addition to removing plaque and tartar with a scaling and root planing procedure, antimicrobial medication placed under the gumline or systemic medications can be used as adjuncts to care to further reduce the bacterial population.
If non-surgical approaches to managing periodontal disease do not achieve the desired outcome, surgery may be recommended to halt its progression and repair damage as possible.
When gum disease has advanced beyond the initial stage, periodontal surgery is often recommended to effectively remove bacteria and tartar from around the teeth, reduce gingival pocket depth, restore lost tissue as possible, and halt disease progression. It’s essential to keep in mind that gum disease is a progressive condition. If appropriate measures are not taken, gum disease continues to compromise the support of the teeth and have consequences to one’s overall dental health and well-being.
As untreated gingivitis evolves into more advanced stages of gum disease, periodontal pockets deepen, the bacteria become more difficult to remove, and the gaps between the surface of the teeth and gums get larger. When pocket depth increases to the point of being beyond the reach of deep cleanings and other conservative methods of care (5mm or more), gum surgery to clean and treat the damage to gums and underlying bone is typically recommended.
The good news is that with proper surgical treatment followed by improved oral hygiene, the chances of tooth loss, further damage to the bone and soft tissues supporting the teeth, and complications from health problems that are linked to periodontal disease can be decreased.
The goals of pocket reduction surgery are to accomplish the following:
Remove sub-gingival bacteria beneath the gums and from the surfaces of the roots of the teeth
Halt damage to the underlying bone, and recontour the affected hard tissues as needed
Reduce pocket depth to facilitate easier cleaning of the teeth and gums and the maintenance of optimal periodontal health
In many cases, a periodontal procedure, which is known as flap surgery, is frequently recommended. During this procedure, the gums in the affected area are reflected away from the teeth and supporting bone. Now, the pocket and roots of the teeth can be thoroughly cleaned and supporting tissues recontoured as needed. When this step gets completed, the tissue flag gets sutured back into place.
Today, in addition to conventional surgical approaches to care, dental lasers are also used to perform select periodontal procedures. When applicable, laser technology can help treat periodontitis, reduce pocket depth, address peri-implantitis, and remove or recontour gingival tissues for cosmetic purposes.
For more information on our office and the many services we provide, give us a call today.
Periodontal disease, commonly called gum disease, is an infection and inflammation of the tissues that surround and support the teeth. It begins when dental plaque and tartar accumulate along the gumline and under the gums, triggering the body’s immune response. Over time this inflammatory process can damage the periodontal ligament and the jawbone that hold teeth in place.
Because early stages of periodontal disease are frequently painless, many people are unaware a problem exists until it progresses. Regular dental exams and periodontal evaluations help identify disease before irreversible damage occurs. Early detection allows for more conservative treatment and better long-term outcomes.
The primary cause of periodontal disease is bacterial plaque, a sticky film that forms on teeth and harbors harmful microbes. Contributing factors include poor oral hygiene, smoking, certain medications, hormonal changes, systemic conditions such as diabetes, and genetic susceptibility. Together, these factors can increase inflammation and speed the breakdown of gum and bone tissue.
Management focuses on removing the bacterial source and addressing modifiable risk factors to slow or stop disease progression. Your dental provider will review medical history and lifestyle factors as part of a comprehensive periodontal assessment. Controlling systemic conditions and quitting tobacco use are often important steps in stabilizing gum health.
Common signs of periodontal disease include red, swollen, or tender gums and bleeding during brushing or flossing. Other warning signs are receding gums, persistent bad breath, tooth sensitivity, looseness of teeth, and new spaces or changes in bite. Any of these symptoms merit a prompt periodontal evaluation to determine the extent of infection and tissue damage.
Because symptoms can be subtle or absent in early stages, regular dental checkups and periodontal probing are essential for people at risk. A professional exam measures pocket depths around teeth and looks for bone loss on radiographs to establish a diagnosis. Early identification increases the likelihood that non-surgical therapy will be effective.
Gingivitis is the earliest, reversible stage of gum disease and is characterized by gum inflammation without loss of the connective tissue or bone that support the teeth. Signs include redness, swelling, and bleeding with brushing, but the underlying periodontal attachment remains intact. With improved home care and professional cleanings, gingivitis can be resolved and progression prevented.
Periodontitis occurs when untreated gingivitis allows inflammation to extend into deeper tissues, causing connective tissue destruction and bone loss. Once attachment and bone are lost, the condition becomes more complex and often requires advanced periodontal treatment to halt progression and attempt to restore support. Distinguishing between these stages guides the treatment plan and long-term maintenance schedule.
Diagnosis begins with a detailed clinical exam that includes measuring pocket depths around each tooth, assessing bleeding on probing, and checking for gum recession and tooth mobility. Dental radiographs are used to evaluate bone levels and detect patterns of bone loss that may not be visible clinically. The clinician will also review medical history and risk factors that influence periodontal health.
Periodic periodontal charting establishes a baseline and helps monitor disease activity over time, which is important for tailoring treatment and maintenance. Laboratory tests or bacterial analyses are sometimes used in complex cases to identify specific pathogens or host-response issues. A comprehensive assessment ensures treatment targets the patient’s particular needs and risk profile.
Non-surgical therapy typically begins with professional mechanical debridement—scaling and root planing—to remove plaque and hardened calculus from beneath the gumline and to smooth root surfaces. This reduces bacterial load and allows inflamed tissues to heal, which often results in decreased pocket depths and improved gum attachment. Adjunctive measures can include localized antimicrobial agents or systemically prescribed medications when indicated.
After initial therapy, personalized oral hygiene instruction and regular periodontal maintenance visits are crucial for long-term success. Many patients respond well to conservative care if they adhere to improved home care and scheduled professional cleanings. When non-surgical treatment does not achieve stability, further evaluation for surgical options may be necessary.
Periodontal surgery is generally recommended when pocket depths remain deep (typically 5 mm or more) despite thorough non-surgical therapy, or when there is significant bone loss that compromises tooth support. Surgical procedures aim to reduce pocket depth, remove inaccessible bacteria, recontour bone and soft tissue, and, when appropriate, regenerate lost tissues. Techniques vary and may include flap surgery, guided tissue regeneration, and bone grafting depending on the clinical goals.
Postoperative care and a structured maintenance plan are essential to preserve surgical outcomes and prevent recurrence. Many surgical approaches are combined with minimally invasive techniques and advanced technologies to enhance healing and patient comfort. Your clinician will explain the recommended procedure, expected healing timeline, and home-care instructions tailored to your situation.
Laser-assisted periodontal therapies can complement conventional treatment by selectively removing diseased tissue, reducing bacterial populations, and promoting a cleaner surgical field in certain procedures. Technologies such as LANAP and other laser protocols are used for pocket decontamination, soft-tissue management, and the treatment of peri-implantitis when clinically appropriate. Lasers may also reduce bleeding and postoperative discomfort for some patients.
While laser treatment offers advantages in select cases, it is not a universal replacement for standard therapies; suitability depends on the type and severity of disease and the clinician’s training. A comprehensive evaluation determines whether laser-assisted therapy is an appropriate adjunct to scaling and root planing or surgical intervention. Discussing expected benefits and limitations with your provider helps set realistic outcomes.
Long-term success depends on consistent daily oral hygiene, including effective brushing, interdental cleaning, and the use of any adjunctive aids recommended by the dental team. Regular periodontal maintenance visits, typically scheduled every three to six months based on disease severity and risk factors, allow professional removal of new plaque and early detection of recurrence. Lifestyle modifications such as quitting tobacco and managing systemic conditions like diabetes also support periodontal stability.
Communication with your dental provider is important to adjust home care routines and maintenance intervals as needed. Using prescribed antimicrobial agents or special rinses may be advised in high-risk situations. Adherence to a personalized prevention plan is the most reliable way to protect the outcomes of periodontal therapy.
Research has established associations between periodontal inflammation and a range of systemic conditions, including cardiovascular disease, diabetes, respiratory issues, and adverse pregnancy outcomes. Chronic oral inflammation can contribute to the body’s overall inflammatory burden, which may influence the course of these conditions. While periodontal treatment does not replace medical care, improving gum health can be an important part of a patient’s overall health strategy.
Because of these links, dental providers routinely review medical history and coordinate care with physicians when systemic concerns are present. Addressing periodontal disease and managing risk factors such as smoking and uncontrolled blood sugar can reduce oral and systemic complications. Patients with chronic medical conditions should inform their dental team so treatment and maintenance plans can be optimized.
To begin, contact the practice to request an appointment for a comprehensive periodontal evaluation and cleaning so the team can assess your current gum health and risk profile. The evaluation typically includes a clinical exam, periodontal charting, and any necessary radiographs to determine the extent of disease and to develop a personalized treatment plan. Preparing a list of medications and relevant medical history will help the clinician provide safe, effective care.
During the visit, the clinician will discuss recommended therapies, expected timelines, and a follow-up schedule to monitor progress. If advanced procedures are indicated, the practice will explain the steps, aftercare, and maintenance needed to support long-term periodontal stability. Patients are encouraged to ask questions so they understand the diagnosis and the rationale for the proposed plan.
