Call Us Today!
(970) 247-2677
New Patients
(970) 233-7384
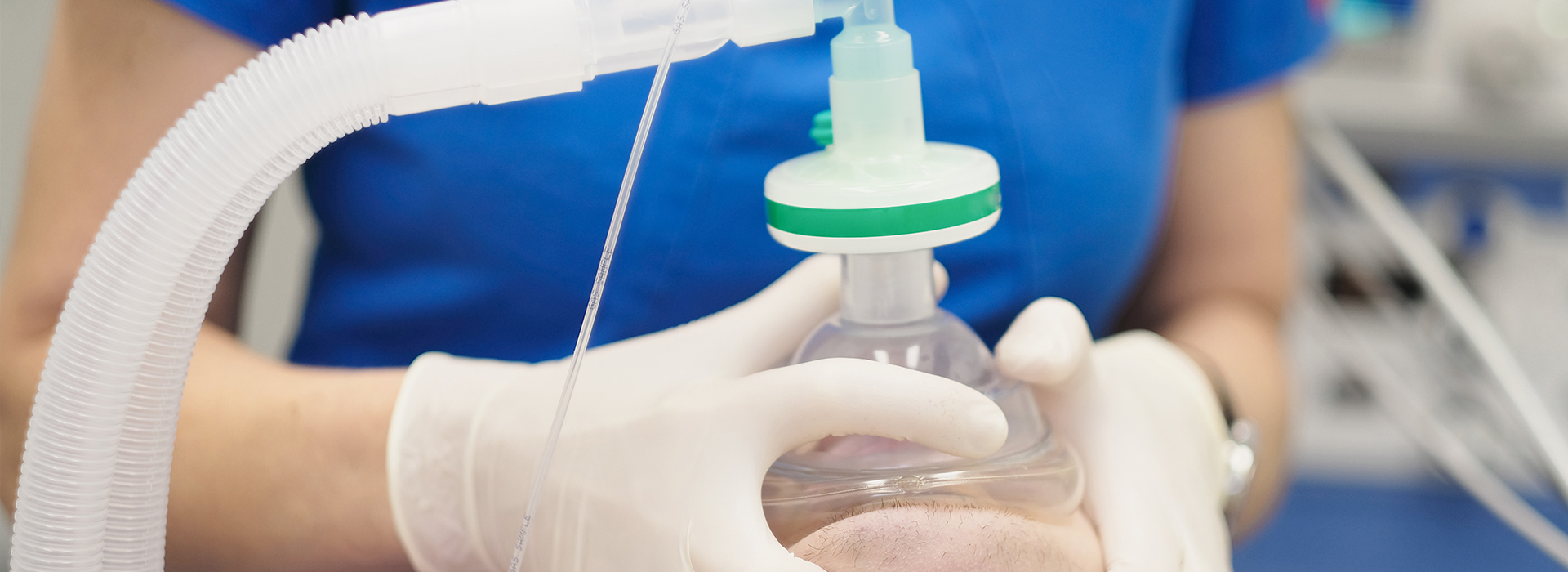
Dental visits can feel stressful for many people — not because dentistry is inherently scary, but because anxiety, sensitivity, and past experiences can turn routine care into something to dread. If you put off checkups or avoid recommended treatments because of nervousness, sedation dentistry offers a clear path back to comfortable, effective care. At Mountain Health Dentistry, our approach focuses on helping you feel calm and secure so you can get the care your smile needs.
Sedation is not about taking control away from you; it’s about giving you options. Carefully chosen, professionally administered sedation techniques help relieve fear, reduce physical discomfort, and make longer procedures manageable — all while letting you remain responsive when appropriate. Our goal is to match the level of sedation to your needs so treatments are safer and easier to receive.
Whether you’ve avoided the dentist for years or simply need help sitting for a specific procedure, sedation dentistry can change how you experience oral healthcare. Below you’ll find straightforward explanations of how sedation works, who typically benefits, and what to expect at each stage of care.
Sedation dentistry creates a calmer environment by using medications that reduce anxiety and promote relaxation. These medications range from mild inhaled agents to oral and intravenous options that provide deeper comfort. The effect is smoother, less stressful appointments for patients who otherwise struggle to tolerate dental treatment.
For many people, sedation reduces the sensory intensity of a dental visit — sounds, smells, and sensations become much less intrusive. This helps patients stay relaxed during procedures that might otherwise provoke tension or movement, improving both safety and the quality of the work performed.
Importantly, sedation is paired with local anesthesia when needed so that you won’t experience pain during treatment. Our team discusses the choices in advance, explains how each option influences awareness and recall, and monitors vital signs throughout the appointment for your safety and comfort.
People opt for sedation for many practical reasons beyond fear alone. Some have an intense aversion to needles, drills, or particular sights and sounds; others have a strong gag reflex or sensitive oral tissues that make routine care painful. Sedation levels the playing field so care can proceed with dignity and minimal distress.
Long or complex appointments are another common reason to consider sedation. When multiple procedures are needed, sedation helps patients stay comfortable through longer visits, which can reduce the number of appointments required and limit overall disruption to daily life.
Sedation can also make treatment possible for individuals who find it hard to sit still — for example, young children with special needs or adults with certain medical or cognitive conditions. With appropriate preparation and monitoring, sedation allows clinicians to provide thorough, efficient treatment where it might otherwise be difficult.
Severe dental fear — for patients whose anxiety prevents them from seeking care, sedation creates a manageable pathway back to oral health.
Procedure-specific anxiety — some treatments provoke more worry than others; sedation can make those particular visits much easier to endure.
Lengthy or multiple procedures — sedation helps patients remain comfortable during extended appointments and can make it practical to complete more work in fewer visits.
Overactive gag reflex — sedation helps reduce gagging, allowing Dr. Miner to work more efficiently while keeping you comfortable.
Heightened sensitivity — patients with very sensitive teeth or oral tissues often benefit from sedation because routine instruments and sensations become more tolerable.
Challenges staying still — children, patients with certain disabilities, or those with medical conditions that limit mobility may receive sedation to facilitate safe, effective care.
Choosing an appropriate sedation strategy begins with a thorough review of medical history, current medications, and the nature of the dental work planned. No single approach suits everyone; our team tailors recommendations so the level of sedation matches each patient’s needs and ensures safe, predictable care.
We discuss expected levels of awareness, how quickly a medication takes effect, and any pre-appointment steps you’ll need to take. This conversation helps you make an informed choice and prepares you for the logistics of the visit, such as whether a companion will need to accompany you afterward.
Monitoring is a core part of safe sedation. Throughout the procedure we track breathing, heart rate, and oxygen levels, and adjustments are made as needed. Our clinicians are trained to respond if a patient requires deeper or lighter sedation at any point during treatment.
Conscious sedation is designed to relax you while allowing you to respond to verbal prompts and breathe on your own. It can range from a light, relaxed state to a deeper level where memory of the procedure may be limited. This approach is commonly used in dental offices because it balances comfort with safety and quick recovery.
General anesthesia, by contrast, produces a deep, controlled state of unconsciousness and is typically administered in a hospital or surgical setting by an anesthesiologist. It’s reserved for cases where other sedation methods are insufficient or when a patient’s medical or psychological needs require that level of support.
Our goal is to use the least invasive option that provides the needed comfort and cooperation. When general anesthesia is recommended, we coordinate with appropriate specialists to ensure care is delivered in the safest possible environment.
Nitrous oxide, commonly called “laughing gas,” is a mild inhaled sedative that reduces anxiety and promotes relaxation. It’s administered through a small mask and combined with oxygen for safety. The gas is discontinued at the end of the appointment and its effects wear off quickly, allowing patients to resume normal activity shortly after treatment.
Oral sedation involves taking a prescribed medication before your visit to reduce anxiety and produce a relaxed state. It’s appropriate for moderate anxiety and some longer procedures. Because these medications can impair alertness, patients usually need an escort to drive them home after the appointment.
IV sedation delivers medication directly into the bloodstream for rapid effect and precise control of sedation level. It’s useful when deeper, adjustable sedation is necessary for complex procedures. IV sedation requires specific pre-appointment instructions, including fasting for a period beforehand, and patients will need someone to accompany them home.
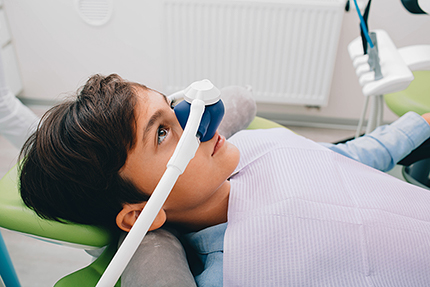
Safety is central to every sedation plan. Before any sedative is administered, our team reviews your health history and current medications, verifies fasting or other preparation instructions, and explains how monitoring will work during your visit. Clear communication helps reduce surprises and increases comfort.
On the day of treatment you’ll be greeted by a team member who reviews the plan, answers questions, and performs a quick assessment. During the procedure, trained staff monitor vital signs and adjust medications as needed. After treatment, you’ll be observed until it’s safe for you to leave with a companion if required.
Recovery varies depending on the type of sedation used. Nitrous oxide typically allows same-day normal activity, while oral and IV sedation may leave residual drowsiness for several hours. We’ll provide care instructions and guidance about when it’s safe to resume routine activities.
Sedation is a tool to help patients receive the dental care they need; it isn’t intended to be a permanent requirement. As treatment progresses, many patients find that once fears are addressed and oral health improves, they become more comfortable with routine visits. We work with you to build a care plan that supports long-term oral health with the least sedation necessary.
Follow-up appointments, preventive care, and a steady relationship with your dental team all contribute to reduced anxiety over time. When additional procedures are needed, we’ll reassess sedation needs and adjust the approach so each visit remains as comfortable and efficient as possible.
If you have particular concerns about sedation or need guidance preparing for an appointment, our team is available to explain options and help you decide on the safest, most comfortable path forward.
In summary, sedation dentistry can make high-quality dental care accessible for patients who would otherwise avoid or delay treatment. For straightforward information about the types of sedation we offer or to discuss whether sedation may be appropriate for you, please contact us for more information.
Sedation dentistry uses medications to reduce anxiety and promote relaxation so patients can receive dental care with less stress. These medications can be delivered through inhalation, orally, or intravenously, and they vary in how quickly they take effect and how deeply they sedate. Sedation is typically combined with local anesthesia to prevent pain while the sedative focuses on comfort and ease of treatment.
The clinical team selects a level of sedation that preserves safety and cooperation while addressing the patient’s needs, ranging from minimal relaxation to deeper, closely monitored states. Monitoring of breathing, heart rate, and oxygen levels is routine during sedated procedures to ensure patient stability. Clear pre-procedure planning and professional oversight help make sedation a predictable way to receive necessary dental care.
Common options include inhaled nitrous oxide for light sedation, prescribed oral medications for moderate relaxation, and intravenous (IV) sedation for rapid, adjustable control of deeper sedation. Nitrous oxide wears off quickly and allows same-day activity in many cases, while oral and IV medications produce more sustained drowsiness and may require an escort home. Each method affects awareness and recovery differently, so choice depends on anxiety level, medical history, and the planned procedure.
Dental teams explain the expected effects of each option so patients understand levels of responsiveness, recall, and recovery time. Patient safety and comfort guide the recommendation, with less invasive options preferred when they adequately meet the clinical need. Proper preparation and monitoring reduce risks and improve the overall experience across all sedation types.
Selecting an appropriate sedation plan begins with a detailed review of medical history, current medications, allergies, and the complexity and duration of the dental work. The clinician evaluates heart and lung health, medication interactions, and any conditions that might affect how a sedative is processed, then discusses realistic expectations and logistics with the patient. Shared decision-making ensures the chosen approach aligns with safety considerations and the patient’s comfort goals.
When necessary, clinicians coordinate with primary care providers or specialists to manage complex medical factors and obtain clearances before proceeding. The team also explains pre-appointment instructions, such as fasting or medication adjustments, so the visit goes smoothly. At Mountain Health Dentistry in Durango, Colorado, this individualized planning helps ensure predictable, patient-centered sedation care.
Sedation dentistry is generally safe when delivered by trained professionals following established protocols for screening, dosing, and monitoring. Safety measures include pre-procedure assessment, continuous monitoring of breathing, heart rate, and oxygenation, and staff trained in airway management and emergency response. Clinics use the minimal effective level of sedation and maintain equipment and medications to respond quickly if adjustments are needed.
Patients are carefully evaluated for conditions that may increase risk, and clinicians modify plans accordingly or refer to a higher-acuity setting when appropriate. Clear communication about medications, recent illnesses, and underlying health issues reduces surprises and helps the team tailor care. Appropriate recovery monitoring and post-procedure instructions further minimize complications and support a safe return to routine activity.
Preparation depends on the type of sedation planned but commonly includes fasting for a specified period before oral or IV sedation and following instructions about routine medications. Patients should bring a list of current medications and medical conditions, arrange for a responsible adult to drive them home if needed, and wear comfortable, loose clothing to the appointment. Avoiding alcohol or recreational drugs before sedation is important and will be reviewed during pre-appointment screening.
The dental team provides written and verbal instructions tailored to the sedation method, and it is essential to follow these directions closely to maintain safety. If you have questions about prescription medications, sleep apnea, pregnancy, or other medical concerns, discuss them ahead of time so the team can adjust the plan. Clear preparation reduces the risk of delays and improves the efficiency and comfort of the visit.
On arrival, a team member reviews the plan, confirms pre-procedure steps, and places monitoring devices to track vital signs throughout the appointment. Sedation is administered according to the chosen method, and staff continually observe responsiveness, breathing, and oxygen levels while local anesthesia is provided if necessary to eliminate pain. Patients may feel drowsy, relaxed, or only mildly aware depending on the sedation level, and sensations such as noise and pressure are usually less intrusive.
After the procedure, patients are observed until it is safe for them to leave; recovery times vary with the type and depth of sedation. Nitrous oxide typically allows rapid return to normal activity, whereas oral and IV sedation often cause residual drowsiness for several hours and require a companion to provide transportation and supervision. The dentist or staff will review aftercare instructions before discharge to support a smooth recovery.
Recovery time depends on the sedation method and individual response: nitrous oxide effects wear off quickly once the gas is stopped, while oral and IV medications can cause drowsiness and impaired coordination for several hours. Patients should plan for a period of rest after deeper sedation and avoid driving, operating machinery, or making important decisions until fully alert. The dental team will advise on when it is safe to eat, take routine medications, and return to work based on the sedative used and your personal reaction.
Alcohol or sedative medications should be avoided for at least 24 hours or according to specific instructions, as combining substances can prolong impairment. If any unusual symptoms such as persistent dizziness, difficulty breathing, or excessive bleeding occur, patients are instructed to contact the dental office or seek urgent care. Clear post-procedure guidance helps patients resume normal activities safely and comfortably.
Yes, with careful evaluation and tailored protocols, sedation can be a safe and effective way to provide dental care for children and patients with special needs who cannot tolerate treatment otherwise. The choice of sedation is influenced by age, weight, medical history, anxiety level, and the type of procedure, and providers follow pediatric or special-needs guidelines to determine the appropriate method. Parental or caregiver consent and clear pre-appointment instructions are essential components of planning for these patients.
Monitoring and staffing are adapted to the needs of pediatric and special-needs patients, and some cases may require collaboration with pediatric anesthesiologists or hospital-based services for higher levels of sedation. Ongoing communication with caregivers about expectations, recovery, and follow-up ensures the best possible outcome. Sedation can make necessary dental treatment achievable while maintaining dignity and minimizing trauma for vulnerable patients.
Levels of sedation influence both awareness and memory: minimal sedation usually preserves full consciousness and recall, moderate sedation may produce drowsiness with limited memory of the procedure, and deeper sedation or general anesthesia can produce little to no memory of events. Many patients appreciate that conscious sedation can reduce anxiety while allowing them to respond to simple prompts, whereas deeper options are chosen when immobility or a complete lack of recall is clinically advantageous. Local anesthesia is used alongside sedation to prevent pain regardless of awareness.
Clinicians discuss the likely degree of recall during the treatment-planning conversation so patients understand what to expect and can provide informed consent. Amnesia can be a desirable effect for highly anxious patients, but it is always balanced with safety considerations and recovery needs. Clear explanation of these effects helps patients choose the option that best matches their comfort goals and recovery preferences.
Sedation is a tool to help patients access necessary dental care and is not intended as a permanent requirement for routine maintenance; many patients find that with treatment, education, and a steady relationship with their dental team they become more comfortable over time. The care plan typically includes follow-up visits, preventive strategies, and a reassessment of sedation needs so that the least invasive option necessary is used for future appointments. Using sedation strategically can reduce the number of visits required to complete treatment while supporting long-term oral health goals.
Before and after sedated procedures, clinicians outline preventive steps and scheduling recommendations to promote healing and minimize further interventions. Each future appointment provides an opportunity to adjust sedation approaches based on past experiences and changing health factors. If you have questions about how sedation could support your dental care, contact Mountain Health Dentistry to discuss options and create a personalized plan.
