Call Us Today!
(970) 247-2677
New Patients
(970) 233-7384
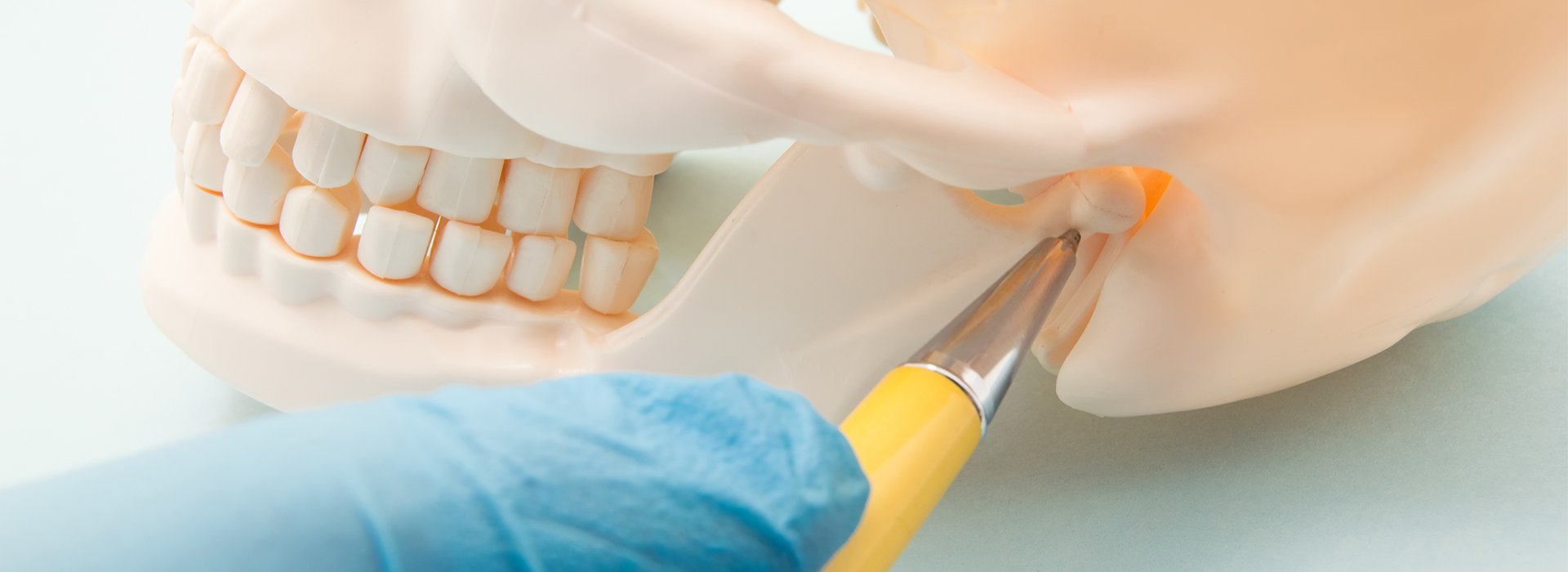
Temporomandibular joint disorders (TMJ disorders or TMD) can affect how you chew, speak, and feel in your face and neck. While many people attribute jaw discomfort to occasional stiffness or stress, persistent or recurring jaw pain often signals a deeper problem in the joint or surrounding muscles. This page explains how the temporomandibular joint works, what commonly causes trouble, how clinicians evaluate TMJ disorders, and the practical treatment and self-care options available to help patients regain comfortable, functional jaw movement. Mountain Health Dentistry approaches TMJ care with a whole-health perspective that emphasizes lasting function and patient comfort.
The temporomandibular joint (TMJ) links the lower jaw to the skull on both the left and right sides, and each joint combines a hinge motion with sliding movements. A small yet resilient disc of fibrocartilage sits between the rounded condyle of the jaw and the temporal bone, cushioning contact and guiding motion. Because the TMJ must coordinate simultaneous up-and-down, forward-backward, and side-to-side movements, it is mechanically complex and relies on precise muscle and ligament balance to function smoothly.
This complexity is what makes the TMJ vulnerable: subtle changes in bite, muscle tension, or disc position can produce significant symptoms. The muscular system that drives the jaw — including the masseter, temporalis, and pterygoid muscles — can react to stress, misalignment, or injury by tightening or spasming, which in turn alters joint loading. Over time, these altered forces may lead to wear of the joint surfaces, disc displacement, or inflammatory changes that perpetuate pain and dysfunction.
Understanding the TMJ’s anatomy helps patients appreciate why symptoms can seem to come from different places. Because the jaw shares nerves with the ear and face, TMJ problems can produce ear-related sensations, facial pain, and headaches — making targeted evaluation essential for accurate diagnosis and effective management.
TMJ disorders present with a wide-ranging symptom profile that can vary from mild and intermittent to severe and persistent. Common symptoms include jaw pain or tenderness, noticeable popping or clicking when opening the mouth, episodes of the jaw locking in an open or closed position, and limitations in how wide a patient can open. Many people also experience related discomfort such as headaches, ear fullness or ringing, neck stiffness, and facial muscle fatigue — symptoms that are sometimes mistaken for other conditions.
Risk factors that increase the likelihood of developing TMJ problems include chronic teeth grinding or clenching (bruxism), prior jaw trauma, certain forms of arthritis, and persistent high muscle tension often related to stress. Dental factors that alter bite relationships, such as missing teeth or uneven restorations, may also contribute by changing the way the jaw closes and distributes force. Recognizing these contributors early can help guide therapy toward reducing harmful joint stress and preventing long-term damage.
Because symptoms overlap with other conditions, patients should be attentive to patterns: symptoms that worsen with jaw use, recur during times of stress, or are accompanied by audible joint noises are more suggestive of a TMJ disorder and warrant professional evaluation. The sooner a patient seeks assessment, the more options are available to manage symptoms conservatively and avoid progression.
Diagnosing a TMJ disorder begins with a careful clinical history and hands-on examination. The clinician will ask about symptom onset, patterns, aggravating and relieving factors, sleep habits, and any history of jaw injury or dental work. A physical exam assesses jaw range of motion, joint sounds, muscle tenderness, bite alignment, and the presence of restrictions or locking. This focused evaluation helps differentiate muscular causes from internal joint issues and from other sources of facial pain.
When indicated, diagnostic imaging supplements the clinical exam. Standard radiographs, panoramic x-rays, or cone-beam computed tomography (CBCT) can reveal structural changes in the joint and surrounding bone. In selected cases, MRI is useful to visualize the joint’s soft tissues — especially the position and condition of the articular disc. These imaging modalities are used selectively, guided by clinical findings, to target the most likely sources of the problem and to inform a personalized treatment plan.
The goal of the diagnostic process is to identify the primary drivers of the symptoms — whether muscular imbalance, disc displacement, degenerative changes, or a combination — so that treatment can be focused and measurable outcomes established. A clear diagnosis also helps set realistic expectations for recovery and maintenance.
Most TMJ disorders respond well to conservative, non-surgical care that aims to reduce pain, normalize jaw function, and protect joint structures. A common first-line intervention is a custom-fitted oral appliance, often called a stabilization splint or night guard, which helps reduce the effects of grinding and can redistribute bite forces to decrease joint strain. These appliances are adjusted to each patient’s bite and used as part of a broader treatment plan.
Complementary in-office approaches may include guided muscle therapies, targeted injections for short-term relief, and occlusal adjustments when specific bite discrepancies contribute to the problem. Dental restorations or orthodontic interventions are considered only when bite-related issues are clearly responsible for ongoing joint stress and when less invasive measures have not resolved symptoms. The practice emphasizes minimally invasive, evidence-based interventions and tailors each plan to an individual’s needs and goals.
When conservative care is insufficient, referral to a specialist for advanced interventions is made thoughtfully and only when those options align with the patient’s clinical situation. Surgical procedures are reserved for persistent internal derangements or severe joint degeneration that produce functional impairment despite thorough non-surgical treatment.
Patients play a central role in managing TMJ conditions. Daily habits that reduce joint load and muscle tension can shorten recovery and lower the chance of recurrence. Recommended measures include eating softer foods temporarily, avoiding wide yawning and prolonged gum chewing, and practicing relaxation techniques to reduce clenching. Simple jaw-stretching routines, when taught by the clinician or a qualified therapist, can help restore mobility and reduce stiffness.
Therapies such as heat or cold applied in short intervals can ease muscle soreness, while over-the-counter anti-inflammatory medications used as directed may provide temporary symptom relief. Behavioral strategies — including awareness of daytime clenching and modifying sleep posture — also contribute to long-term improvement. For patients with significant bruxism, collaboration with dental professionals to design protective appliances and with medical providers when sleep-related issues are suspected is often helpful.
Successful long-term management combines clinical care with patient-led strategies and periodic reassessment. Regular follow-up ensures that treatments are adjusted as needed and that any emerging issues are addressed early, preserving jaw function and quality of life over the long term.
In summary, temporomandibular joint disorders encompass a range of conditions that can be effectively evaluated and managed with a combination of careful diagnosis, conservative therapies, and patient-centered self-care. The practice at Mountain Health Dentistry takes a measured, whole-health approach to help patients restore comfortable jaw movement and maintain long-term function. If you would like more information about TMJ evaluation or treatment, please contact us to discuss your concerns and next steps.
Temporomandibular joint disorders, often called TMJ disorders or TMD, refer to problems that affect the jaw joint and the muscles that control jaw movement. These conditions can involve the joint’s cartilage disc, the bony surfaces, the surrounding ligaments, or the muscles that open and close the jaw. Because the TMJ combines hinge and sliding motions, even small changes in any component can alter how the joint functions and cause pain or limited movement.
TMJ disorders range from short-term muscle pain to longer-term internal joint derangements or degenerative changes. Symptoms can fluctuate in intensity and may affect one or both sides of the face, making accurate assessment important for effective management. Early recognition and targeted care help preserve joint function and reduce the risk of chronic symptoms.
Common signs that warrant an evaluation include persistent jaw pain or tenderness, repeated clicking or popping during jaw movement, episodes of jaw locking, and difficulty opening the mouth fully. Many patients also report related symptoms such as frequent headaches, ear fullness or ringing, facial pain, and neck tension that accompanies jaw use. Symptoms that worsen with chewing, increase during stress, or recur over time are particularly suggestive of a TMJ disorder.
If symptoms interfere with eating, speaking, sleep, or work activities, a professional assessment is recommended to identify the underlying cause and begin appropriate treatment. Early assessment broadens conservative care options and can limit the chance of progression to more complex joint problems. A focused clinical exam helps distinguish TMJ-related pain from other sources of facial or ear discomfort.
TMJ problems most commonly stem from a combination of muscular tension, parafunctional habits such as teeth grinding or clenching, and changes in how the teeth meet when the jaw closes. Trauma to the jaw, inflammatory joint disease, and certain degenerative conditions can also alter joint mechanics and lead to symptoms. In many cases, multiple contributing factors interact—for example, stress-related clenching can worsen a preexisting disc displacement or arthritic change.
Dental factors such as missing teeth, uneven restorations, or sudden changes in bite can change joint loading and precipitate symptoms when the system is already vulnerable. Sleep-disordered breathing and certain medical conditions that affect muscle tone or connective tissues may increase susceptibility to TMJ issues. A comprehensive evaluation considers all of these potential contributors to develop an individualized treatment plan.
Diagnosis begins with a detailed history and hands-on examination that assesses jaw range of motion, joint sounds, muscle tenderness, and bite relationships. The clinician will ask about symptom patterns, triggers, sleep habits, prior injuries, and any dental treatments that might affect jaw function. This focused clinical assessment helps differentiate muscular pain from internal joint derangement and identifies signs that indicate the need for further testing.
When indicated by clinical findings, imaging tools supplement the exam to clarify joint structure and soft tissue position. Panoramic radiographs or cone-beam computed tomography (CBCT) can show bony changes, while magnetic resonance imaging (MRI) is the preferred study to visualize disc position and soft tissue inflammation. Imaging is used selectively and interpreted in the context of the clinical picture to guide targeted treatment decisions.
The goal of the diagnostic process is to identify the primary drivers of symptoms—muscle imbalance, disc displacement, degenerative change, or a combination—so that treatment can be tailored and progress monitored. A clear diagnosis also helps set realistic expectations for recovery and outlines strategies for long-term maintenance of jaw health.
The majority of TMJ disorders are managed successfully with conservative, non-surgical approaches that focus on reducing pain and restoring normal function. Typical first-line measures include behavioral modification to reduce clenching, short-term use of anti-inflammatory medications as directed, and application of heat or cold to relieve muscle soreness. Supervised jaw exercises and physical therapy techniques can help normalize movement and reduce muscular tension.
Custom oral appliances, targeted manual therapies, and occlusal adjustments when appropriate are often integrated into a comprehensive plan to protect joint structures and redistribute forces. In-office interventions such as guided muscle therapy or short-term injection techniques may provide additional relief for selected patients. The emphasis is on evidence-based, minimally invasive care tailored to the individual’s needs and monitored for measurable improvement.
Custom-fitted dental appliances, commonly called stabilization splints or night guards, are designed to reduce the harmful effects of grinding and clenching by altering how the teeth contact and by cushioning forces on the joint. These appliances can relax overactive muscles, decrease parafunctional tooth contact, and provide a more stable jaw position that reduces joint strain. They are made from dental impressions or digital scans to ensure a precise fit and are adjusted to each patient’s bite.
Appliances are typically part of a broader treatment plan and are used in conjunction with behavioral strategies and therapeutic exercises. Some patients benefit from daytime devices when clenching is frequent, while others use night guards primarily to protect teeth and minimize nocturnal bruxism. Regular follow-up is important to adjust the appliance and evaluate symptom response over time.
Dental restorations, extractions, orthodontics, and other procedures that change how the teeth meet can influence jaw mechanics and potentially affect TMJ symptoms. When bite relationships are altered significantly, the distribution of forces across the joint and muscles may change, which can either alleviate preexisting stress or, in some cases, reveal underlying dysfunction. Good clinical practice evaluates TMJ status before extensive rehabilitation and addresses occlusal factors only when they clearly contribute to symptoms.
When bite-related issues are believed to be a primary driver of TMJ pain, conservative occlusal adjustments or targeted restorative treatments may be considered as part of a coordinated plan. These interventions are chosen selectively after thorough assessment and often after conservative therapies have been attempted. Collaborative care with specialists may be recommended for complex cases that require multidisciplinary planning.
Self-care plays a central role in short-term relief and long-term management of TMJ disorders. Practical measures include eating softer foods temporarily, avoiding gum chewing and wide yawning, practicing conscious relaxation to reduce daytime clenching, and using short applications of moist heat or cold to ease muscle soreness. Gentle, clinician-recommended jaw-stretching and mobility exercises can help restore range of motion and reduce stiffness.
Behavioral techniques such as limiting stimulants before bed, improving sleep posture, and developing stress-management habits can reduce parafunctional activity that aggravates the joint. For patients with significant nighttime grinding, a custom appliance made by a dental professional offers protection while other strategies address underlying contributors. Ongoing communication with the care team ensures self-care is safe and effective for each individual.
Referral to a specialist or consideration of surgical options is appropriate when patients have persistent internal joint derangement, severe degenerative changes, or ongoing functional impairment despite a thorough course of conservative care. Signs that may prompt referral include progressive loss of jaw opening, persistent locking, worsening joint degeneration on imaging, or failure to achieve meaningful improvement after structured non-surgical treatment. Specialists can offer advanced diagnostic evaluation and discuss the risks and benefits of further interventions.
Surgical procedures are reserved for specific, well-delineated conditions and are considered only after careful multidisciplinary assessment and conservative attempts have been exhausted. When surgery is indicated, the goal remains to restore function, reduce pain, and improve quality of life, with postoperative rehabilitation to support long-term outcomes. Thoughtful selection of candidates and clear communication about expected results are essential parts of the process.
The practice takes a whole-health, patient-centered approach that begins with a detailed history and focused clinical exam to identify the primary drivers of a patient’s symptoms. Conservative, evidence-based therapies are prioritized, including custom-fitted oral appliances, guided muscle treatments, therapeutic exercises, and targeted in-office interventions when appropriate. Imaging is used selectively to clarify structural concerns and to tailor care to each individual’s needs.
Mountain Health Dentistry emphasizes restoring comfortable function and preventing long-term damage through coordinated care and ongoing follow-up. Patients are encouraged to participate actively in self-care and behavioral strategies while the clinical team monitors progress and adjusts treatment as needed. This measured approach helps preserve jaw health and supports durable, patient-specific outcomes.
