Call Us Today!
(970) 247-2677
New Patients
(970) 233-7384

We accept patient self-referrals and referrals from other dentists.
Apical surgery — commonly called an apicoectomy or root-end surgery — is a targeted procedure that addresses persistent infection or inflammation at the very tip of a tooth’s root. It becomes an appropriate choice when standard root canal therapy has not resolved symptoms or when anatomic factors prevent complete cleaning from inside the root canal system. The goal is conservative: remove the diseased tissue at the root tip and seal the root so the natural tooth can remain functional in the mouth.
This operation is precise and purpose-driven. Rather than removing the entire tooth, the clinician works through a small incision in the gum to access the root end, excise the infected portion, and place a biocompatible seal. Because the approach focuses on the root tip and surrounding bone, it avoids more extensive surgery and gives patients a real opportunity to keep their natural tooth when retreatment alone is unlikely to succeed.
At Mountain Health Dentistry, we prioritize treatments that conserve tooth structure and protect overall oral health. Dr. Miner evaluates each case with modern imaging and clinical examination to determine whether apical surgery offers the best balance of long-term success, comfort, and preservation of function.
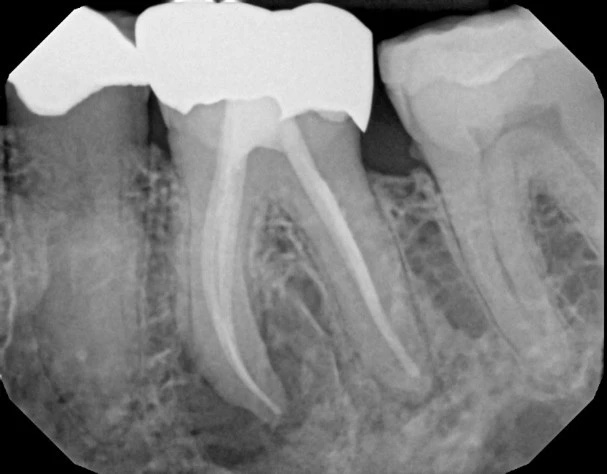

The images above illustrate typical intraoperative perspectives and anatomic views relevant to root-end procedures. They are intended to show how focused the access is and how only a small portion of the root and surrounding tissue is addressed during the operation. Individual anatomy and clinical findings vary, so visual examples are for general orientation rather than an exact representation of any single patient’s experience.
Before any incision is made, the tooth and surrounding area are numbed thoroughly with local anesthesia, and sedation is available when indicated to support patient comfort and reduce anxiety. The surgeon creates a small flap in the gum to expose the underlying bone and root. A precise window in the bone grants direct access to the root tip so the diseased tissue can be removed under magnification, often using surgical microscopes or loupes for greater accuracy.
Once the root tip is visible, the surgeon trims the infected portion and prepares the root end for sealing. A retrograde filling material is placed at the root end to create a durable seal that prevents bacteria from re-entering the canal system. The gum tissue is then repositioned and sutured to promote predictable healing. The entire procedure is usually completed in a single appointment; how long it takes depends on the tooth and surrounding anatomy.
Modern apical surgery emphasizes microsurgical techniques and materials that reduce trauma and improve outcomes. Clinicians use sterile technique, magnification, and refined instruments to minimize tissue disruption, which often leads to less postoperative discomfort and faster recovery compared with older, more invasive methods.
After apical surgery, most patients experience some localized swelling and mild discomfort for a few days. Pain is typically manageable with over-the-counter analgesics or short courses of prescribed medication when necessary. Cold compresses, gentle oral hygiene around the surgical site, and adherence to post-operative instructions help control swelling and support healing. Sutures are usually removed or dissolve within about a week depending on the material used.
Bone and soft tissues remodel over weeks to months. Initial healing of the soft tissue often occurs within two weeks; bone maturation and complete resolution of the radiographic signs of infection can take several months. Follow-up visits allow your clinician to monitor progress, check the seal at the root end, and verify that symptoms have resolved. If healing proceeds as expected, the tooth can remain a comfortable, functional part of the mouth for years to come.
Complications are uncommon but may include prolonged discomfort, delayed healing, or the need for further intervention if residual infection persists. Careful case selection, imaging, and surgical technique reduce these risks. If any concerns arise during recovery, prompt communication with the dental team ensures issues are addressed quickly and conservatively.
Apical surgery is one of several ways to address a tooth that remains symptomatic after root canal therapy. In some cases, nonsurgical retreatment of the root canal — reopening the tooth, removing past filling materials, and thoroughly disinfecting and re-sealing the system — is a better first step when the root canal anatomy is accessible and the clinician believes the source of the problem can be reached from inside the tooth.
If the tooth is structurally compromised beyond repair or if repeated efforts are unlikely to provide a durable solution, extraction and tooth replacement options such as implant-supported restorations or bridges may be discussed. These are valid options in certain clinical scenarios, and the decision-making process balances the desire to preserve natural teeth against long-term predictability, function, and patient preferences.
Your clinician will review all suitable options, including the likely benefits and limitations of each approach. Treatment planning for a tooth with a persistent root issue often involves imaging, clinical assessment, and a frank discussion about what will best protect oral health and function over time.
We believe in a conservative, evidence-informed approach that places a high value on preserving natural teeth whenever clinically appropriate. Saving a tooth with careful endodontic and surgical management can maintain chewing function, aesthetics, and bone support without the need for more extensive reconstructive work. This philosophy guides our recommendations and the technologies we use to improve precision and comfort.
Advanced imaging, magnification, and minimally invasive surgical techniques allow our team to address complex root-end problems with greater predictability. Dr. Miner and the clinical staff collaborate to tailor treatment to each patient’s anatomy, health history, and goals. When apical surgery offers the best chance of maintaining a natural tooth, we focus on doing the procedure with meticulous attention to technique and postoperative care.
Ultimately, preserving a healthy, pain-free tooth is the preferred outcome when it aligns with long-term oral health. We aim to give patients clear, unbiased information so they can make informed decisions, supported by clinical expertise and a commitment to conservative care.
If you have persistent tooth pain, swelling, or a history of a root canal that has not fully resolved, contact us to discuss whether apical surgery may be appropriate for your situation. Our team is available to review imaging, explain the options, and recommend a care plan aimed at keeping you comfortable and preserving your natural teeth when possible. Please contact us for more information about apical surgery and other tooth-preserving treatments.
Apical surgery, often called an apicoectomy or root-end surgery, is a targeted procedure that treats infection or inflammation at the tip of a tooth root. The operation focuses on removing diseased tissue around the root end and sealing the canal from the outside to prevent bacteria from re-entering. The primary goal is to preserve the natural tooth and restore comfort and function when nonsurgical endodontic treatment is unlikely to resolve the issue.
The approach is conservative compared with extraction and replacement because only a small portion of root and surrounding tissue is addressed. Microsurgical techniques and magnification allow clinicians to work through a small gum incision and a precise bone window. Using biocompatible retrograde filling materials, the root is sealed to promote long-term healing of the surrounding bone and soft tissue.
Apical surgery is usually considered when symptoms persist after root canal therapy or when anatomic factors prevent complete cleaning of the canal system from inside the tooth. It may be recommended when previous nonsurgical retreatment is unlikely to reach the source of infection, when a canal is blocked by posts or calcification, or when a perforation or complex anatomy limits success of internal retreatment. Clinical signs such as localized pain, swelling, or radiographic evidence of a persistent lesion prompt evaluation for a surgical option.
Deciding among apical surgery, nonsurgical retreatment, or extraction involves careful imaging and clinical assessment. Modern imaging such as CBCT helps define root anatomy and the extent of bone involvement to guide the recommendation. Your clinician will review the probable benefits, limitations, and expected outcomes of each option so you can choose the approach that best protects long-term oral health.
The procedure begins with local anesthesia and, when appropriate, sedation to ensure patient comfort. The surgeon creates a small flap in the gum to expose the bone, then makes a precise opening in the bone to access the root tip; magnification and microsurgical instruments are typically used to enhance accuracy. The infected portion of the root is removed, the root end is prepared, and a retrograde filling material is placed to seal the canal from the root end.
After the root end is sealed, the soft tissue flap is repositioned and sutured to support predictable healing. The entire procedure is often completed in a single appointment, though duration varies with tooth location and complexity. Sterile technique, refined instruments, and advanced materials aim to minimize tissue trauma and support a rapid, comfortable recovery.
It is common to experience mild to moderate swelling and some discomfort for a few days after surgery, which is generally managed with over-the-counter pain relievers or a short course of prescribed medication if needed. Cold compresses, rest, and gentle oral hygiene around the surgical site help control swelling and reduce the risk of irritation. Patients are usually advised to avoid strenuous activity, follow a soft diet for a short period, and return for any scheduled follow-up visits.
Sutures may dissolve or be removed about a week after the procedure depending on the material used, and soft tissue healing often progresses significantly within two weeks. Bone remodeling and complete resolution of radiographic signs of infection can take several months, so periodic follow-up imaging is important to confirm full healing. If unusual or worsening symptoms occur, contacting the dental team promptly helps address any concerns early.
Apical surgery carries risks similar to other minor oral surgical procedures, including infection, prolonged swelling, delayed healing, bleeding, or temporary changes in sensation near the surgical area. Less commonly, the procedure may not fully resolve the infection, necessitating further treatment or alternative options such as extraction. Careful case selection, surgical technique, and sterile protocol reduce the likelihood of complications.
Some teeth have anatomic considerations that raise the complexity of surgery, such as proximity to nerves or sinus cavities, and these factors are evaluated with imaging beforehand. Your clinician will discuss any specific risks related to your anatomy and health history and explain steps taken to minimize them. Prompt communication during recovery ensures that any unexpected developments are addressed quickly and conservatively.
When performed with modern microsurgical techniques and proper case selection, apical surgery has a high success rate for resolving persistent root-end infections and preserving the natural tooth. Factors that influence success include the tooth's anatomy, the extent of bone loss, the presence of complex canal systems, the quality of prior root canal treatment, and overall patient health. Using magnification, advanced materials, and sterile technique improves the likelihood of durable healing.
Long-term success also depends on appropriate postoperative care and the absence of new sources of reinfection, such as recurrent decay or coronal leakage. Regular dental checkups and good oral hygiene support the longevity of the treated tooth. In cases where predictable healing is less likely, the clinician will discuss realistic expectations and alternative options so patients can make informed decisions.
Preparation typically involves a clinical exam and imaging, such as digital radiographs or CBCT, to assess the root anatomy and surrounding structures. Your clinician will review your medical history, current medications, and any conditions that might affect healing, and may recommend temporary medication adjustments in coordination with your physician when necessary. Preoperative instructions often include planning for a ride home if sedation is used and arranging a short period of rest after the procedure.
Following specific instructions about eating, medication use, and oral hygiene on the day of surgery helps reduce complications and improve comfort. If you have concerns about anxiety or pain control, discuss sedation options ahead of time so the team can tailor the approach to your needs. Clear communication with the dental team ensures that expectations are set and that you arrive prepared for a smooth appointment.
Yes. Nonsurgical retreatment of the root canal is often the first alternative, involving reopening the tooth, removing old filling materials, thoroughly disinfecting the system, and resealing the canals. Retreatments can be highly effective when the canal anatomy is accessible and the source of infection can be reached internally. The choice between retreatment and apical surgery depends on whether internal access can adequately address the problem and on anatomic factors revealed by imaging.
When neither retreatment nor surgery offers a predictable long-term solution, extraction and replacement with an implant-supported restoration or bridge may be considered. Those options provide reliable function and aesthetics in many cases, but they involve different procedures and timelines and are selected based on overall oral health and patient goals. Your clinician will present the appropriate alternatives and explain how each option aligns with your priorities.
When healing proceeds as expected, apical surgery can restore comfort and preserve the tooth so it functions normally for many years. Success depends on complete sealing of the root end, adequate supporting bone, and prevention of new sources of contamination such as recurrent decay or a failed coronal restoration. Proper restoration of the tooth after surgery and ongoing oral hygiene are important contributors to maintaining long-term function.
Regular follow-up appointments and periodic imaging allow the dental team to monitor healing and detect any changes early, which supports durable outcomes. In some situations additional restorative work or monitoring is needed to ensure the tooth remains stable. Your clinician will outline a follow-up plan tailored to the tooth and your overall oral health needs.
The practice emphasizes a conservative, evidence-informed approach that prioritizes preserving natural teeth when clinically appropriate. Cases are evaluated with modern imaging and magnification to determine whether apical surgery offers the best balance of long-term success, comfort, and preservation of function. Minimally invasive microsurgical techniques and sterile protocols are used to reduce tissue trauma and support predictable healing.
At Mountain Health Dentistry in Durango, our team collaborates to tailor treatment plans to each patient's anatomy, health history, and goals, and we provide clear explanations about expected outcomes and recovery. Follow-up care and open communication are integral parts of the process so concerns are addressed promptly and healing is monitored until the tooth is stable. Patients can expect a focus on precision, comfort, and tooth-preserving solutions throughout their care.
