Call Us Today!
(970) 247-2677
New Patients
(970) 233-7384

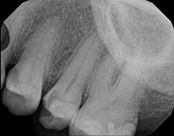
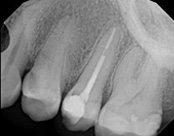
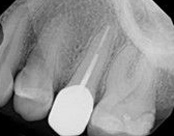
The patient presented with mild pain, a cavity, and a broken filling was evident. After performing diagnostic testing, the diagnosis was: irreversible pulpitis, symptomatic periradicular periodontitis. Root canal therapy was done and the tooth healed well and is still functioning.
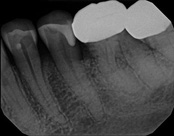
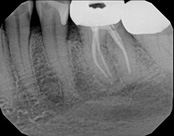
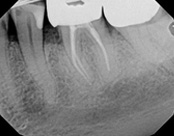
This patient presented with pain when chewing. Diagnostic testing was done and determined it was the lower molar. The diagnosis was: pulpal necrosis, symptomatic periradicular periodontitis. Root canal treatment was performed with laser disinfection. The tooth had a crown and we accessed the tooth through the crown. We saved the tooth and the crown.
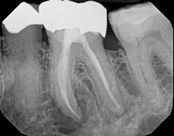
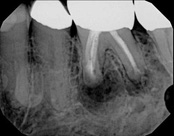
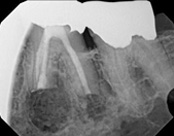
This person saw a specialist and was told the molar tooth needed to be extracted because the root canal failed and was infected. The root canal had been done by an endodontic specialist. The diagnosis was: previous endodontic treatment, chronic periradicular abscess. We did an apicoectomy and saved the patient’s tooth.
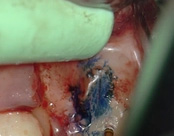
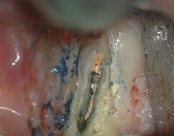
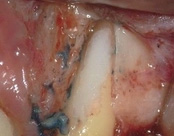
The patient was eating and bit down, felt and heard a “pop.” The tooth had cracked in the middle of the root. The tooth helps hold the patients partial in place and did not want to lose the tooth. The crack was removed with the laser and then restored.
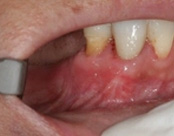
The photograph is 2 months after the crack repair. The area looks like nothing was done (no redness, no scarring, etc.) and the tooth is there helping to hold the partial denture.
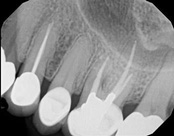
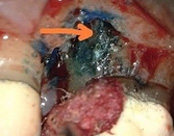
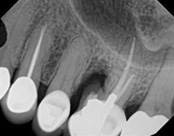
This patient had root canal treatment many, many years ago. One root developed a crack all the way through the root leading to an abscess. That root was removed and the tooth is still functionable.
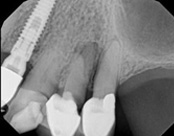
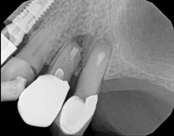
In this situation, some would say the canals are so “calcified” that root canal treatment can’t be done; or sometimes the canal can’t be found. And because of that the tooth would need an extraction and an implant. In some instances, root canal therapy can’t be done but that does not mean the tooth is a loss. The solution is micro-apical surgery, an apicoectomy.
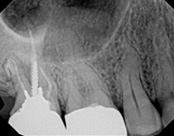
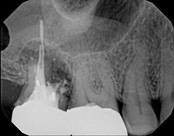
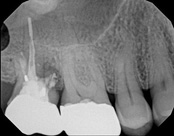
This person had root canal therapy many years ago. One root had excess material outside of the root preventing healing. Another root had a perforation (a hole) and a crack. The large root had a post and had not healed from the initial root canal treatment.
The post was removed, that root was retreated. The root with the excess material, an apicoectomy was done, the excess material, and infection cleaned out. The root with the perforation and crack was removed. The tooth healed and is still in function. This area is a poor area for an implant.
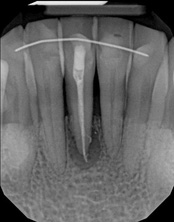
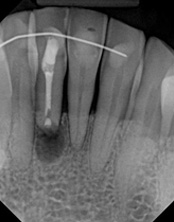
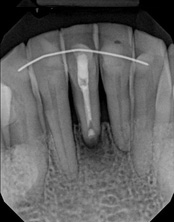
The patient was told by a specialist that the root canal failed, the only option was extraction and an implant. She did not want to do that; she wanted to keep her tooth, after all, it is her front tooth. She found us. We performed an apical microsurgery with the laser. The tooth was saved and is still functioning. This is a poor area for an implant, so much better to save the tooth.
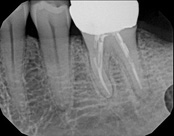
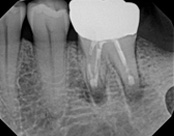
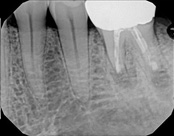
This patient presented with a failed root canal. The root canal became infected. An apicoectomy (apical microsurgery) was performed using the laser. Patient had minimal swelling, minimal discomfort, and fast healing. The tooth was saved and an implant avoided. This tooth tends to have a lower success rate with root canal therapy; thankfully apical microsurgery was available to save the tooth.
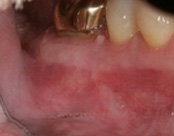
At the 3 month follow-up, the gums look like nothing was done thanks to the skill and use of the laser for the procedure.
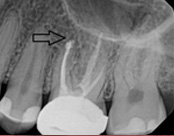
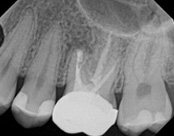
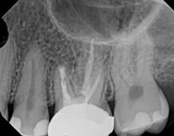
This person presented with one root that had failed from root canal treatment. The arrow in the picture, shows the infection as well as extra filling material that was pushed out of the root. An apical microsurgery was performed using the laser. The infection and excess material was cleaned out. Complete healing is visible 3 months after. The tooth was saved. This is a poor area for an implant.
The gallery serves as an educational library of clinical images and procedural descriptions that illustrate common tooth-preserving techniques and dental technologies. It is intended to help patients better understand the types of treatments offered and the clinical considerations that guide care. The gallery emphasizes clinical information rather than personal endorsements or outcome guarantees.
The content focuses on procedures, tools, and general healing patterns so visitors can learn what to ask about during a consultation. Images and captions are organized to clarify terminology and to show how different technologies are used in practice. This resource is designed to support informed conversations with your dental team.
The gallery highlights a range of tooth-preserving procedures, including endodontic treatments such as root canal therapy and root canal retreatment, apical microsurgery (apicoectomy), root amputation, mid-root crack management, and laser-assisted disinfection. It also references adjunctive technologies like laser dentistry, CBCT imaging, and intraoral scanning that support diagnosis and treatment planning. Each entry focuses on the clinical rationale and the role of those techniques in preserving natural teeth when appropriate.
Descriptions emphasize the indications for each approach and the types of clinical issues they address, such as persistent infection, complex anatomy, calcified canals, or structural compromise of a root. The intent is to provide context about why a clinician might recommend one procedure over another, rather than to predict individual outcomes. Readers can use this information to prepare questions for their provider.
Clinical images are captured using standard dental photography practices and digital imaging systems to ensure clarity and clinical usefulness. Radiographic and three-dimensional images may be included when they add diagnostic value; captions explain the imaging modality and what clinicians evaluate. Photographs are cropped and annotated as needed to focus attention on the relevant clinical features and technologies rather than extraneous detail.
Text accompanying each image explains the procedure type, the tools used, and the clinical considerations that informed treatment decisions. The presentation aims for clear, factual descriptions that support patient education and shared decision-making. Materials are curated to reflect typical clinical scenarios, not to serve as case endorsements.
Patient privacy and consent are integral to the use of clinical images in any educational gallery. Images shown publicly are used only after obtaining documented permission from patients, and identifying details are removed or obscured to the extent required by privacy regulations. The practice follows applicable privacy standards to protect patient information in both clinical records and public materials.
Where necessary, images are de-identified so that individuals cannot be recognized from the published content. Consent processes typically include an explanation of how images will be used and the opportunity for patients to decline. Patients who have questions about image use are encouraged to discuss them with the clinical team prior to providing permission.
The gallery provides general information about typical healing patterns and the clinical signs clinicians monitor during follow-up, such as soft-tissue appearance, resolution of symptoms, and radiographic signs of bone healing. Descriptions explain common post-procedure expectations like transient soreness, gradual tissue remodeling, and the timeline for clinical reassessment. This helps patients understand the usual course of recovery without implying a guaranteed result for every individual.
Information also covers how technologies such as lasers and microsurgical techniques can influence inflammation and soft-tissue response in clinical settings. Patients are reminded that individual healing varies according to health status, the complexity of the condition, and adherence to post-operative instructions. For personalized guidance, a clinical evaluation is necessary to set realistic expectations for recovery.
Captions and labels in the gallery are intended to clarify common dental terms and procedural names, such as apicoectomy, pulpal necrosis, retreatment, and laser disinfection. Each label explains the core meaning in plain language and identifies the clinical issue being addressed, as well as the general goal of the procedure. Brief definitions help bridge the gap between technical terminology and patient understanding.
If you encounter unfamiliar terms, the gallery encourages noting them and bringing questions to your consultation. Clinicians can explain how a given term applies to your specific situation and why a particular technique may be recommended. This approach supports clearer communication and better-informed decision-making.
The gallery is an educational tool that outlines the types of tooth-preserving treatments that may be considered for various clinical problems, but it is not a substitute for a personalized clinical evaluation. The decision between extraction and tooth-saving therapy depends on multiple factors, including the extent of structural damage, the health of surrounding tissues, bone support, the patient's overall health, and long-term restorative planning. Visual examples and procedural descriptions can help you understand options that a clinician might discuss.
Ultimately, appropriate treatment selection requires diagnostic tests, clinical examination, and a discussion of goals and risks with your dentist or specialist. Use the gallery to prepare questions about the feasibility, risks, and benefits of different approaches so you can participate in an informed treatment decision. Your provider will tailor recommendations to your unique clinical circumstances.
The gallery is curated by the clinical team with oversight from the practice lead and licensed clinicians who are responsible for ensuring clinical accuracy and appropriate educational context. Images and captions undergo review to verify that procedural descriptions reflect accepted clinical standards and the technologies listed are used in accordance with professional guidelines. This editorial process helps maintain the gallery as a reliable educational resource.
Clinical staff update entries when new technologies or protocols are adopted, and peer review within the practice helps ensure consistency and clarity. If viewers have questions about clinical content, the team encourages them to raise those questions during an appointment for a personalized explanation. Professional accountability is a core principle in maintaining the gallery's usefulness.
Updates to the gallery occur as the practice adopts new techniques, documents representative clinical scenarios, or determines that additional educational material would benefit patients. The clinical team evaluates potential additions for educational value, relevance to common clinical questions, and compliance with privacy and consent policies. Photographic quality and clear explanatory text are prerequisites for inclusion.
New content is also informed by advances in diagnostic imaging, changes in standard-of-care protocols, and feedback from clinicians about topics patients commonly ask about. The goal is to keep the resource current and aligned with clinical best practices so patients can access meaningful educational material. Periodic review ensures older entries remain accurate and clearly explained.
Use the gallery as a way to familiarize yourself with common procedures and terms so you can have a more productive conversation with Dr. Miner. Take note of items that spark questions, such as specific techniques or technologies you would like explained, and bring your past dental records and imaging if available. Doing so enables Dr. Miner to relate gallery content to your unique situation and provide targeted guidance.
Prepare a list of practical concerns to discuss, such as the diagnostic steps Dr. Miner will use, proposed follow-up plans, and how treatment fits into your overall dental and medical history. If you would like to review gallery material in person, mention it when scheduling an appointment so the team can allocate time to address your questions. Patients visiting Mountain Health Dentistry in Durango can review gallery examples with Dr. Miner during a consultation to help clarify treatment options.
