Call Us Today!
(970) 247-2677
New Patients
(970) 233-7384
Being told a tooth needs a root canal can be unsettling, but modern root canal therapy is a reliable way to relieve pain while preserving the natural tooth. When the inner tissues of a tooth are infected or irreversibly damaged, removing the source of disease and restoring the tooth’s function usually leads to better long-term outcomes than losing the tooth and replacing it later. The focus is practical: stop the infection, save structure, and return you to comfortable chewing and smiling.
At Mountain Health Dentistry we combine contemporary instruments and a patient-centered approach to make root canal care efficient and predictable. Our team emphasizes clear explanations, gentle technique, and thoughtful follow-up so you understand what’s happening and feel confident about your treatment. We aim to protect your oral health with treatments that are evidence-based and aligned with your overall wellbeing.
Keeping a natural tooth whenever possible preserves the tooth’s role in biting, chewing, and maintaining the alignment of neighboring teeth. A live or successfully treated tooth continues to support the surrounding bone and gum tissue; removing it, even with a good replacement option, changes the biomechanics of the mouth and can create new challenges over time.
Root canal therapy is a conservative solution because it removes infected tissue from inside the tooth while leaving the outer tooth intact. That preserved structure is easier to restore with a crown or onlay than it is to replace a missing tooth later. In other words, saving the tooth often reduces the amount of additional restorative work required down the road.
Success rates for modern root canal treatment are high when diagnosis is accurate and the tooth receives appropriate final restoration. Our clinical goal is to restore both comfort and long-term function so you can eat, speak, and enjoy daily life without worrying about recurring problems.
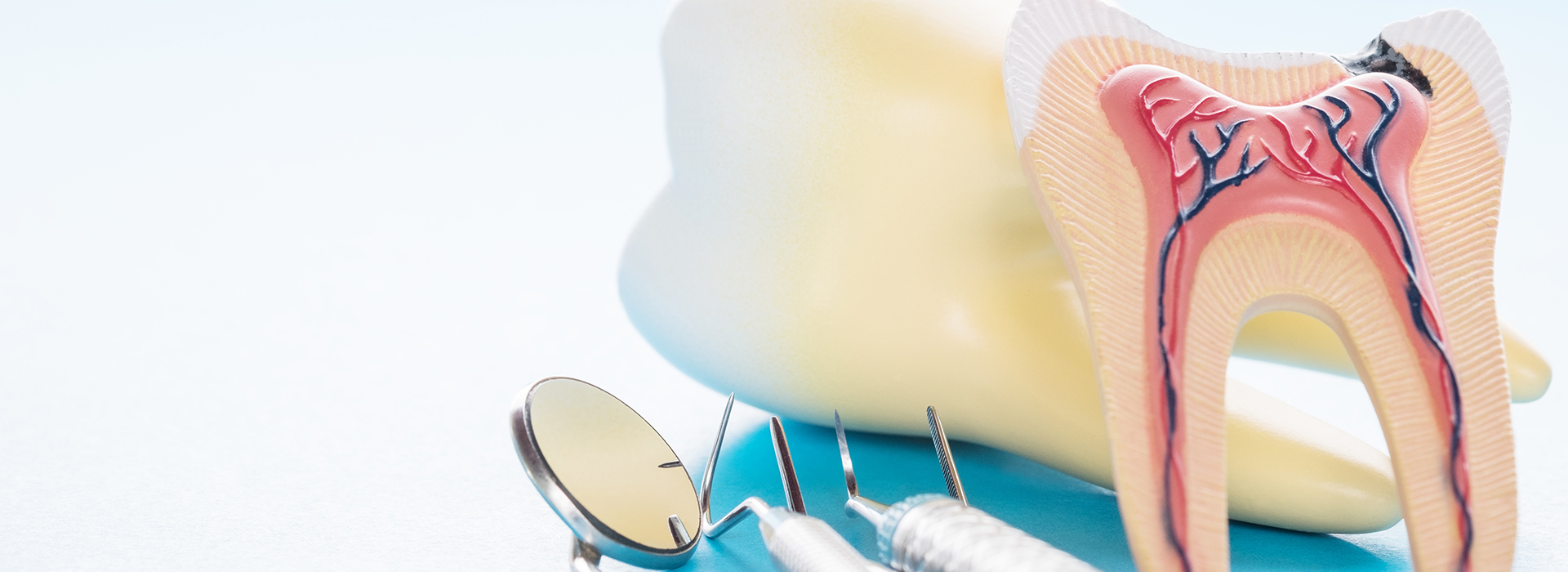
Each tooth contains a central chamber that once housed living pulp tissue — nerves, blood vessels, and connective tissue. While an adult tooth can remain functional without living pulp, that internal chamber communicates with the rest of the tooth through narrow root canals. When bacteria reach the chamber through deep decay, a crack, or an injury, they can inflame or infect the pulp.
Infection may begin with fleeting sensitivity to hot, cold, or sweets and progress to persistent pain or swelling. Sometimes the tooth becomes discolored or a small bump appears on the gum, indicating drainage from an internal infection. Because symptoms vary widely — from intense, sudden pain to almost no obvious discomfort — careful clinical and radiographic assessment is essential to identify the problem early.
Root canal therapy addresses the issue by removing the diseased tissue, disinfecting the canals, and sealing the space to prevent reinfection. Prompt, accurate diagnosis and treatment reduce the chance that the infection will damage surrounding bone or spread to adjacent teeth.
Persistent pain that grows worse with time, interrupts sleep, or reacts strongly to pressure often points to inflammation inside the tooth. Any toothache that doesn’t resolve quickly should be evaluated to determine whether the pulp is involved.
When brief sensitivity becomes prolonged or severe, it may indicate the pulp is irritated or infected. These changes in sensitivity are an early warning sign that professional attention is needed.
Discomfort on biting can mean the tooth’s internal support has been compromised, sometimes because of a crack that reaches the pulp or because infection has weakened the surrounding tissues.
A tooth that becomes gray or darker after injury or prolonged decay may have lost vitality. Discoloration is a visible clue that the internal tissues might be compromised.
Cracks and chips can open a path for bacteria to enter the pulp. Treating the interior of the tooth often makes it possible to preserve what remains of the natural structure with a well-fitting restoration.
Localized swelling or a recurring pimple on the gum near a tooth is frequently a sign that infection has reached the root tip and is trying to drain. These findings call for timely evaluation and treatment.
Infections that affect the supporting bone can lead to increased mobility. Treating the source at the root often allows the tissues to heal and stability to return.
Intervening before infection spreads usually makes treatment simpler and more predictable. When a root infection is small and confined to the canal system, a standard root canal and an appropriate restoration will often resolve the issue with minimal follow-up. Left unchecked, the infection can erode bone, create chronic drainage, or cause damage that requires more complex procedures.
Delaying care can turn a straightforward root canal into a case that needs retreatment, surgical intervention at the root tip, or ultimately extraction. Early diagnosis allows clinicians to tailor a conservative plan that preserves as much natural tooth and tissue as possible.
Our team discusses anticipated steps, timing for a final restoration, and indicators to watch for during healing. That transparent planning helps patients make informed choices and reduce the likelihood of unexpected complications.
Thanks to advances in tools and infection-control protocols, root canal appointments today are far more comfortable and efficient than in the past. Most cases are treated with local anesthesia so the tooth is numb during the procedure; if needed, calming aids such as nitrous oxide or oral sedation are available to help anxious patients relax.
Treatment begins by isolating the tooth and creating a small access point to the pulp chamber. The clinician uses specialized instruments and antimicrobial irrigants to clean and shape the canals, removing diseased tissue and bacteria. Once the canals are dry and disinfected, a biocompatible material seals the space to block future contamination.
Some teeth can be completed in a single visit; others require multiple appointments because of complex anatomy or active infection that benefits from interim medications. After the root canal is finished, a durable restoration — commonly a crown — is recommended to protect the treated tooth and restore full function.
It’s normal to feel mild soreness around a tooth for a few days after treatment as the surrounding tissues settle. Over-the-counter pain relievers typically manage this discomfort effectively; if prescription medication is needed, it will be provided. We give clear aftercare instructions so you know what to expect and how to protect the tooth while it heals.
Because a treated tooth may be more brittle until it receives its permanent crown or onlay, it’s wise to avoid very hard or sticky foods on that side. Completing the recommended restoration in a timely manner reduces the risk of fracture and extends the life of the treatment.
Antibiotics are used only when clinically necessary. Routine follow-up visits and occasional radiographs help confirm that the area around the root is healing and that the tooth remains stable. With proper restoration and home care, a tooth that has had root canal therapy can function successfully for many years.

At Mountain Health Dentistry our focus is relieving pain, controlling infection, and restoring strength and function so you can return to your normal routine. If you’re experiencing symptoms or want to know whether root canal therapy is the right option for a specific tooth, please contact us for more information and to schedule an evaluation.
A root canal is an endodontic procedure that removes inflamed or infected pulp tissue from inside a tooth, disinfects the canal system, and seals the space to prevent reinfection. By addressing the source of infection while preserving the outer tooth structure, the procedure allows the natural tooth to remain functional for biting and chewing. Modern root canal therapy focuses on eliminating disease and restoring comfort so patients can avoid unnecessary extractions.
Keeping a natural tooth whenever feasible helps maintain proper alignment, distribute biting forces, and support surrounding bone and gum tissue. After the canal system is sealed, a durable restoration such as a crown or onlay is typically placed to protect the treated tooth and restore full function. With appropriate restoration and follow-up, a treated tooth can remain stable and useful for many years.
Common signs that a tooth may need root canal therapy include persistent or worsening tooth pain, prolonged sensitivity to hot or cold, pain when biting, and swelling or a small bump on the gum near the affected tooth. A tooth that darkens in color after an injury or shows increased mobility can also indicate internal damage or infection. Symptoms vary widely, and some infected teeth produce minimal discomfort while still posing a risk to surrounding tissues.
Because symptoms can be subtle or mimic other problems, a careful clinical exam and radiographs are essential to determine whether the pulp is involved. Early evaluation helps prevent the spread of infection and often keeps treatment more straightforward. If you notice any of these signs, prompt assessment reduces the chance of more complex procedures later.
Diagnosis begins with a thorough clinical examination that may include percussion and palpation tests, cold and electric pulp testing, and visual assessment for cracks or deep decay. Dental radiographs, and when indicated three-dimensional imaging such as CBCT, provide critical information about root anatomy and the presence of periapical infection. Combining clinical findings with imaging helps clinicians differentiate pulp disease from other causes of dental pain.
Sometimes symptoms require careful correlation to rule out referred pain or periodontal issues, and additional tests help clarify the source of discomfort. Once the diagnosis is established, the dentist outlines a treatment plan that considers tooth anatomy, restorability, and the patient’s overall health. Accurate diagnosis guides predictability and helps set realistic expectations for healing.
Modern root canal treatment usually begins with local anesthesia to ensure comfort, followed by isolation of the tooth to prevent contamination. The clinician creates a small access opening, uses specialized instruments and antimicrobial irrigants to clean and shape the canals, and removes diseased tissue and bacteria. Once the canal system is disinfected and dried, a biocompatible filling material seals the space to block future infection.
Some teeth can be completed in a single visit while others need multiple appointments when anatomy is complex or an active infection benefits from interim medication. After the root canal is finished, the tooth is restored with a protective restoration—commonly a crown or onlay—to restore strength and function. The dentist will review follow-up timing and signs to watch for as the tooth heals.
Thanks to modern anesthetics and techniques, most root canal procedures are performed with minimal discomfort during the appointment, and many patients report little to no pain. Postoperative soreness in the surrounding tissues is common for a few days but is usually manageable with over-the-counter pain relievers and recommended aftercare. If prescription medication is needed for discomfort, the clinician will provide appropriate guidance.
For patients who experience anxiety, calming aids such as nitrous oxide or oral sedation are available to enhance comfort and reduce stress during treatment. Your dentist will discuss sedation options, expected effects, and any pre-appointment instructions to ensure a safe, comfortable experience. Clear communication about your comfort preferences helps the team tailor care to your needs.
Recovery after a root canal typically involves mild soreness that decreases over several days as surrounding tissues settle and inflammation resolves. It is advisable to avoid very hard or sticky foods on the treated side until the permanent restoration is placed, since a recently treated tooth can be more brittle. Maintaining good oral hygiene and following the aftercare instructions provided by your clinician supports healing and reduces the risk of complications.
Complete restoration with a crown or onlay should be scheduled in a timely manner to protect the tooth from fracture and restore full function. Routine follow-up visits and occasional radiographs allow the dentist to verify that the bone and surrounding tissues are healing properly. If swelling, persistent pain, or other unexpected symptoms occur, contact your dental office for evaluation.
After root canal therapy the tooth has often lost some internal structure and can be more prone to fracture, so a crown or onlay is recommended to restore strength and protect the remaining tooth. A well-fitting restoration redistributes biting forces and seals the tooth against reinfection, helping ensure long-term success of the endodontic treatment. Without an appropriate final restoration, the treated tooth is at higher risk of structural failure.
The choice between a crown and an onlay depends on how much natural tooth structure remains and the location of the tooth in the mouth. Your dentist will evaluate the tooth and discuss restorative options that balance preservation of tooth structure with durability. Timely coordination between endodontic treatment and restorative care improves outcomes and reduces the need for future intervention.
When diagnosis is accurate and the tooth receives appropriate cleaning, sealing, and final restoration, modern root canal treatment has high success rates and reliably relieves pain and infection. Risks include persistent or recurrent infection, missed canals, fracture of the tooth, or rare complications related to complex anatomy. Most issues can be managed predictably with retreatment or adjunctive procedures if they occur.
Several factors influence outcomes, including the presence of preexisting infection, canal anatomy, the quality of the restoration, and the patient’s overall health and oral hygiene. Regular follow-up and timely restoration are important contributors to long-term success. Your dentist will explain realistic expectations and the factors that most affect prognosis for your specific tooth.
Retreatment is considered when a previously treated tooth develops new symptoms, radiographic signs of persistent infection, or when the original filling did not adequately seal all of the canal anatomy. Root canal retreatment involves re-entering the canal system to remove old material, disinfect, and reseal the canals. It is often successful when the cause of failure is a missed canal, inadequate obturation, or reinfection.
Apical surgery, also called root end surgery, may be recommended when retreatment is not feasible or when an infection persists at the root tip despite nonsurgical efforts. This procedure addresses disease at the root apex directly and preserves the remaining tooth when appropriate. The dentist will review diagnostic imaging, including CBCT when needed, to determine the most conservative and predictable option.
At Mountain Health Dentistry we emphasize evidence-based, tooth-preserving care that combines advanced diagnostics and gentle technique to achieve predictable results. Our team uses modern imaging and precise instrumentation to identify complex anatomy, control infection, and plan coordinated restorative care that restores long-term function. Clear communication and personalized treatment planning help patients understand each step and expected outcomes.
We prioritize comfort and safety by offering effective local anesthesia and calming options, and we collaborate closely with patients and restorative dentists to ensure timely crowns or onlays after treatment. This approach supports durable healing and helps protect natural teeth whenever possible, preserving oral health and daily function for years to come.
