Call Us Today!
(970) 247-2677
New Patients
(970) 233-7384
We accept patient self-referrals and referrals from other dentists.
Root-end surgery — commonly called an apicoectomy — is a targeted surgical option for teeth that continue to show signs of infection or inflammation after conventional root canal therapy. Instead of immediately removing a problematic tooth, this procedure treats the source of the problem at the root tip, aiming to preserve the tooth’s natural structure and function. For many patients, that approach keeps daily life and oral function undisturbed while protecting long-term oral health.
The decision to recommend root-end surgery is clinical and individualized. It takes into account factors such as the condition of the existing root canal treatment, anatomical considerations visible on advanced imaging, the patient’s overall oral health goals, and the relative benefits of conserving the natural tooth versus extraction and replacement. Our team prioritizes clear explanations so patients can make informed choices about their care.
Root-end surgery becomes a consideration when nonsurgical retreatment is unlikely to resolve an ongoing problem or when retreatment has already failed. Common reasons include a persistent infection at the root tip, a fractured root that prevents complete canal cleaning, a blocked or calcified canal that cannot be negotiated, or an unusual root anatomy that leaves residual bacteria in areas that cannot be reached with conventional treatment.
Symptoms that may prompt evaluation include lingering or recurrent pain, swelling, a draining sinus tract, or radiographic evidence of a radiolucency at the root apex. However, some troublesome lesions are discovered incidentally on routine imaging; lack of symptoms does not always mean absence of disease. Advanced imaging such as cone beam CT (CBCT) provides a three-dimensional view that helps clinicians determine whether apicoectomy is technically feasible and likely to be successful.
Where appropriate, the course of care may include nonsurgical retreatment first, followed by surgical intervention if necessary. The goal is always to choose the least invasive, most predictable approach that preserves oral health and long-term function.
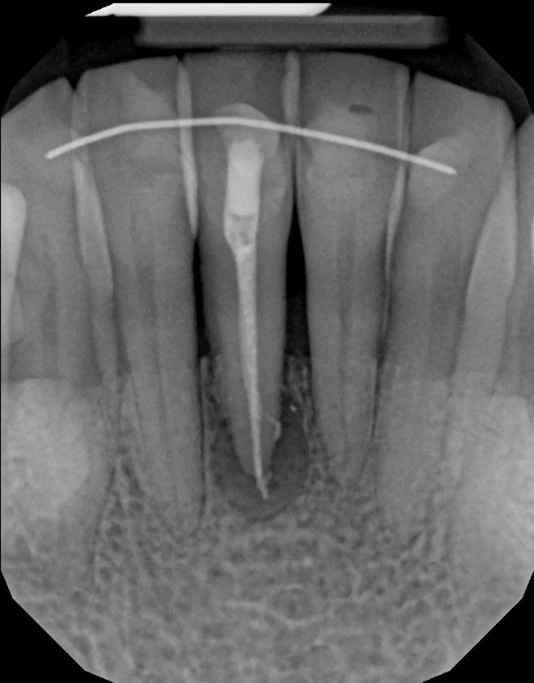
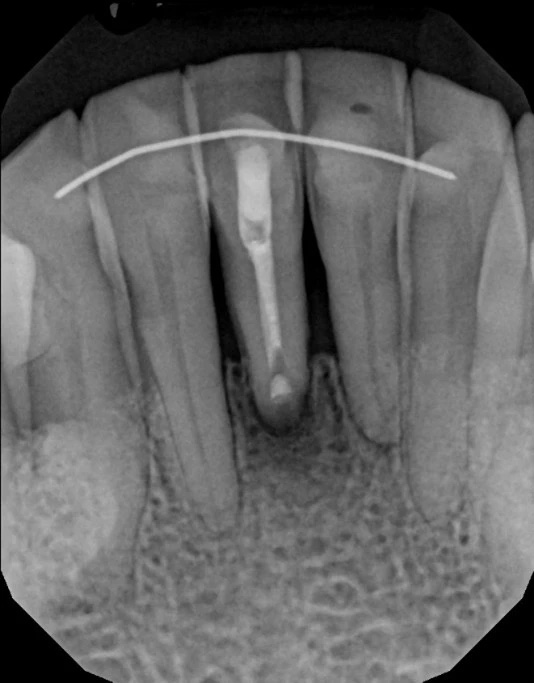
An apicoectomy is a precise surgical procedure that removes the diseased tissue at the tip of a tooth root and seals the root end to prevent reinfection. The clinician gains access to the root tip through a small incision in the gum, removes a few millimeters of the root end along with any surrounding infected tissue, and places a biocompatible seal — often referred to as a root-end filling — to close the canal from the root tip side. This retrograde seal helps isolate the root canal system from surrounding tissues.
Modern techniques emphasize microsurgical approaches that use magnification and fine instruments to conserve bone and soft tissue. Microsurgery improves visualization of complex anatomy, allows for smaller incisions, and supports more predictable tissue handling. In many cases, a successful apicoectomy preserves the tooth for years while eliminating symptoms and radiographic signs of infection.
Determining candidacy for apicoectomy involves careful assessment of the tooth’s restorability, the quality of the existing root canal filling, and the tooth’s strategic value in the mouth. When anatomy, prior treatment, or anatomic obstacles limit the effectiveness of nonsurgical methods, apicoectomy can be a durable alternative to extraction.
The procedure begins with local anesthesia to ensure patient comfort; sedation options may be available for patients with dental anxiety. The clinician makes a small incision in the gum tissue near the affected tooth and gently reflects the tissue to expose the underlying bone. A tiny window is made in the bone to reveal the root tip and any adjacent lesion. Using magnification and microinstruments, the infected root tip and surrounding granulation tissue are carefully removed.
After the diseased material is excised, the root canal is inspected from the root end and a retrograde filling is placed to seal the canal. Contemporary materials used for this purpose are designed to be biocompatible and to create a long-lasting barrier against bacterial infiltration. The gum tissue is repositioned and sutured; sutures are typically removed within a week, and most patients experience a relatively rapid return to routine activities when recovery is well managed.
Because apicoectomies are conservative by design, the procedure often takes less than an hour for a single-rooted tooth, though complexity and the number of roots involved can extend that time. The use of microscopes, microsurgical instruments, and advanced imaging contributes to more precise outcomes and improved healing trajectories.
Initial healing after root-end surgery involves a predictable period of soreness and mild swelling that typically resolves within several days. Clinicians provide specific aftercare instructions that commonly include measures to control swelling, guidelines for eating and oral hygiene, and recommendations for over-the-counter pain relief. Antibiotics may be prescribed when clinically indicated, but they are not a routine part of every case.
Patients are usually advised to avoid chewing on the treated side for a short time, to maintain gentle oral hygiene around the surgical area, and to attend a follow-up appointment so the clinician can evaluate soft-tissue healing and remove sutures. Radiographic follow-up over the ensuing months is important to confirm bone healing at the root tip; while soft tissue often heals quickly, bone remodeling and complete resolution of a lesion can take several months.
Long-term success depends on a combination of surgical technique, the quality of the retrograde seal, and the overall restorative plan for the tooth. When the surgical site heals and the canal remains sealed, many patients retain comfortable, functional teeth without need for extraction or prosthetic replacement.
One of the primary advantages of root-end surgery is tooth preservation. Maintaining a natural tooth preserves the surrounding bone, supports adjacent teeth, and often delivers the most natural chewing and esthetic outcomes. In appropriate cases, apicoectomy avoids the need for extraction and the subsequent restorative steps that replacement would require.
That said, apicoectomy is not always the best choice. Anatomical constraints, widespread root fractures, insufficient remaining tooth structure, or an inability to obtain a predictable seal may make extraction and replacement (such as with an implant or bridge) the more reliable long-term solution. Nonsurgical retreatment of the root canal is often considered first; when retreatment is not feasible or fails, surgery can be the next step.
Clinical decision-making is collaborative and evidence-based. Our team coordinates diagnostic imaging, evaluates restorative considerations, and discusses realistic expectations so patients know the potential benefits and limitations of each option. When indicated, root-end microsurgery is a conservative, focused procedure that can extend the life of a tooth and preserve oral health.
Mountain Health Dentistry approaches these cases with an emphasis on preservation, modern imaging, and minimally invasive technique to give patients the best chance of retaining their natural teeth.
In summary, root-end surgery is a precise, conservative surgical option designed to remove infection at the root tip and preserve a natural tooth when nonsurgical approaches are insufficient. If you have concerns about a persistent root canal problem, ongoing discomfort, or imaging that suggests a persistent lesion, please contact us to learn more about whether this treatment is right for you.
Root-end surgery, commonly known as an apicoectomy, is a focused surgical treatment that addresses persistent infection or inflammation at the tip of a tooth root after conventional root canal therapy. The procedure removes diseased tissue at the root apex and places a biocompatible retrograde filling to seal the canal from the root end. This approach aims to preserve the natural tooth when nonsurgical retreatment is unlikely to resolve the problem.
Modern apicoectomies use microsurgical techniques, magnification, and fine instruments to conserve bone and soft tissue and to improve visualization of complex anatomy. Because the surgeon works directly at the root tip, the procedure can eliminate localized sources of infection while maintaining surrounding structures. When successful, root-end surgery helps patients retain a functional, natural tooth for years to come.
Root-end surgery is considered when nonsurgical retreatment is unlikely to succeed or has already failed to eliminate signs of infection at the root tip. Indications include a persistent radiolucency at the apex, a fractured or blocked canal that cannot be negotiated, or unusual root anatomy that leaves residual bacteria after standard treatment. Symptoms prompting evaluation may include lingering pain, swelling, or a draining sinus tract, although some lesions are found incidentally on imaging.
Clinical decision-making balances the tooth’s restorability, strategic value in the mouth, and the likelihood of predictable healing with surgical intervention. Advanced imaging such as cone beam CT (CBCT) helps determine whether apicoectomy is technically feasible and likely to succeed. The goal is always to choose the least invasive, most reliable option that preserves oral health and long-term function.
Cone beam CT provides a three-dimensional view of the tooth, surrounding bone, and nearby anatomical structures, enabling more precise diagnosis and surgical planning. CBCT can reveal canal morphology, root fractures, the extent of periapical lesions, and relationships to critical structures such as sinuses or nerves. This detailed information helps clinicians assess whether a retrograde approach is feasible and what surgical access will be required.
Using CBCT reduces uncertainty during case selection and supports microsurgical strategies that minimize bone removal and protect adjacent anatomy. The technology improves communication with patients by showing the problem in three dimensions and explaining why a particular course of care is recommended. Ultimately, CBCT contributes to more predictable outcomes and tailored treatment plans.
The apicoectomy typically begins with local anesthesia and, if desired or indicated, sedation options to ensure patient comfort. The clinician makes a small incision in the gum to expose the underlying bone, creates a tiny window in the bone to visualize the root tip, and carefully removes the diseased root end and surrounding granulation tissue. After inspecting the canal from the root end, a biocompatible retrograde filling is placed to seal the canal and prevent reinfection.
Microsurgical instruments and magnification enable smaller incisions, more precise tissue handling, and conservative bone management. The gum tissue is repositioned and sutured, with suture removal typically occurring within a week, and radiographic follow-up scheduled to monitor bone healing. Procedure time varies with complexity but many single-rooted teeth can be treated in under an hour when performed with modern microsurgical techniques.
Initial recovery after root-end surgery commonly involves mild to moderate soreness, some swelling, and sensitivity that generally improve within a few days to a week. Clinicians provide specific aftercare instructions such as cold compresses, gentle oral hygiene measures around the surgical site, and recommendations for over-the-counter analgesics when appropriate. Antibiotics are prescribed only when clinically indicated, rather than routinely.
Patients are usually advised to avoid chewing on the treated side briefly and to attend a follow-up visit for suture removal and soft-tissue evaluation. Radiographic monitoring over the next several months is important to confirm bone remodeling and lesion resolution, since complete bone healing can take time. Adhering to postoperative guidelines and attending follow-up appointments supports predictable long-term outcomes.
As with any surgical procedure, apicoectomy carries risks such as temporary discomfort, swelling, infection, or delayed healing, and rare complications involving adjacent anatomical structures. Microsurgical methods and careful imaging assessment reduce these risks by improving precision and limiting tissue disturbance. Success rates vary depending on tooth anatomy, prior treatment quality, and the presence of complicating factors like root fractures, but many studied cases show favorable long-term outcomes when cases are selected appropriately.
Long-term success depends on the quality of the retrograde seal, the surgical technique, and the overall restorative plan for the tooth. Teeth with complex anatomy or structural compromise may have a lower probability of success and require close monitoring or alternative restorative strategies. Collaborative planning between the surgeon and restorative dentist helps set realistic expectations and optimize the tooth’s prognosis.
Nonsurgical retreatment is often considered first because it addresses the entire canal system from the crown and can be less invasive than surgery. Root-end surgery becomes a preferred option when retreatment is unlikely to reach the area of infection due to blocked canals, complex anatomy, or procedural limitations. Extraction and replacement with an implant or bridge may be recommended when the tooth is structurally unsalvageable or when surgical and nonsurgical approaches are unlikely to provide a predictable outcome.
The choice among these options is individualized and evidence-based, weighing the tooth’s functional importance, remaining tooth structure, patient preferences, and long-term prognosis. When a tooth can be predictably preserved, apicoectomy often offers the benefits of maintaining natural tooth function and supporting surrounding bone. Shared decision-making and thorough diagnostic workups guide patients to the most appropriate care path.
Good candidates for apicoectomy are patients whose teeth have persistent apical pathology that cannot be resolved through conventional nonsurgical retreatment or when retreatment is technically infeasible. Candidates typically have adequate tooth structure for restoration, localized lesions at the root tip, and an overall oral health status that supports healing. Patients with uncontrolled systemic conditions may require medical clearance or stabilization before undergoing surgery.
A thorough clinical exam and advanced imaging are essential to confirm candidacy, evaluate anatomical constraints, and plan a conservative surgical approach. The clinician also considers the tooth’s strategic value in the mouth and the patient’s long-term oral health goals. When selected appropriately, apicoectomy can be a durable, tooth-preserving alternative to extraction.
Yes, root-end surgery is specifically valuable in cases with complex root anatomy, calcified or blocked canals, and prior treatment where conventional access cannot fully address the infected area. By approaching the canal system from the root tip, the clinician can remove the infected portion and place a retrograde seal in locations that are otherwise unreachable. Microsurgical techniques and enhanced visualization are particularly helpful in managing unexpected anatomy while minimizing bone removal.
In some situations a fractured root or extensive structural damage limits the tooth’s long-term prognosis despite successful apicoectomy, so careful assessment is necessary. The combined expertise of endodontic and restorative clinicians helps determine whether the tooth can be predictably restored after surgery. When feasible, the microsurgical approach often extends the functional life of teeth that would otherwise be at high risk for extraction.
At Mountain Health Dentistry in Durango, Colorado, our approach emphasizes preservation, modern imaging, and minimally invasive microsurgical techniques to give patients the best chance of retaining natural teeth. We integrate CBCT imaging and magnification to plan each case carefully and to tailor the surgical approach to the tooth’s anatomy and the patient’s overall oral health goals. Patient comfort and clear communication are priorities throughout diagnosis, treatment, and follow-up.
Our team coordinates with restorative providers and follows evidence-based protocols to monitor healing and long-term success, including scheduled radiographic follow-up to confirm bone remodeling. We discuss all appropriate options so patients can make informed decisions about preservation versus extraction and replacement. When root-end surgery is indicated, the emphasis is on precise technique, conservative tissue handling, and predictable outcomes.
